The expenses associated with receiving rehabilitative treatment from a licensed therapist within a patient’s residence encompass various factors, including the therapist’s credentials, the duration and frequency of sessions, the geographic location, and the specific needs of the individual. For instance, a patient recovering from surgery might require more intensive and specialized care than someone managing a chronic condition.
Providing therapeutic interventions in a familiar and comfortable environment offers several potential advantages. This approach can reduce travel time and associated costs, especially for individuals with mobility challenges. It can also foster a more personalized therapeutic relationship, allowing the therapist to tailor exercises and strategies to the patient’s unique home environment. Historically, such personalized care was often reserved for the affluent, but advancements in healthcare accessibility have made it a more viable option for a broader population.
This article will delve deeper into the various components influencing these expenses, exploring strategies for managing them effectively and highlighting the potential long-term value of this personalized approach to healthcare.
Tips for Managing Expenses Related to Receiving Physical Therapy at Home
Managing the financial aspects of receiving rehabilitative treatment within one’s residence requires careful planning and consideration. The following tips offer guidance for navigating these expenses effectively.
Tip 1: Verify Insurance Coverage: Contact insurance providers to determine the extent of coverage for at-home therapeutic services. Policies vary significantly, and pre-authorization might be required.
Tip 2: Explore Package Deals: Some providers offer discounted rates for multiple sessions purchased in advance. This can be a cost-effective strategy for individuals requiring ongoing care.
Tip 3: Consider Telehealth Options: Virtual consultations can supplement in-person sessions, potentially reducing overall costs while still providing valuable guidance and support.
Tip 4: Negotiate Rates: Discuss pricing options with potential providers. Some therapists offer sliding scales based on financial need or may be open to negotiating fees.
Tip 5: Inquire About Equipment Rentals: If specialized equipment is necessary, explore rental options rather than purchasing outright, potentially saving significant upfront costs.
Tip 6: Explore Community Resources: Local community centers or non-profit organizations may offer subsidized or free therapeutic services for eligible individuals.
Tip 7: Maximize Home Exercise Programs: Actively participating in prescribed home exercises can improve recovery time and potentially reduce the number of sessions required.
By implementing these strategies, individuals can effectively manage expenses while maximizing the benefits of personalized rehabilitative care in the comfort of their homes. These practices empower patients to take an active role in their recovery journey while navigating the financial aspects of care.
The following section will conclude this discussion by summarizing the key takeaways and highlighting the importance of proactive planning in healthcare decisions.
1. Therapist's Credentials
A therapist’s credentials significantly influence the cost of in-home physical therapy. Higher credentials often reflect greater expertise and specialized training, typically commanding higher fees. Understanding these qualifications allows patients to assess the value proposition in relation to their individual needs.
- Degrees and Licenses:
Therapists hold varying degrees, from a Doctor of Physical Therapy (DPT) to a Master of Physical Therapy (MPT) or a Bachelor of Science in Physical Therapy (BSPT). Licensure is mandatory for practice and ensures adherence to professional standards. While all licensed therapists provide essential care, those with doctoral degrees may possess advanced knowledge in specific areas, potentially justifying higher session rates.
- Board Certifications:
Board certification demonstrates advanced competency in specialized areas, such as geriatrics, neurology, or orthopedics. Therapists holding these certifications have undergone rigorous examinations and demonstrate expertise in their chosen fields. This specialized knowledge can result in more effective treatment, often reflected in higher fees.
- Years of Experience:
Experience significantly influences cost. Seasoned practitioners often charge more due to their accumulated knowledge and refined skills. While newer graduates may offer lower rates, extensive experience frequently correlates with improved diagnostic abilities and treatment efficacy.
- Continuing Education:
Commitment to continuing education demonstrates a therapist’s dedication to staying current with the latest advancements and techniques. This ongoing professional development can enhance treatment outcomes, sometimes justifying higher costs for patients seeking cutting-edge care.
Ultimately, selecting a therapist involves balancing credentials, experience, and cost. While higher qualifications often correlate with higher fees, specialized expertise can lead to more effective treatment and potentially faster recovery. Careful consideration of these factors ensures patients receive optimal care that aligns with their individual needs and budgetary considerations.
2. Session Duration
Session duration is a pivotal factor influencing the overall cost of in-home physical therapy. The length of each session directly correlates with the total expense, impacting treatment plans and budget considerations. Understanding the nuances of session duration empowers patients to optimize their care while managing financial constraints effectively.
- Standard Session Lengths:
Typical in-home physical therapy sessions range from 30 to 60 minutes. Shorter sessions may focus on specific exercises or modalities, while longer sessions allow for more comprehensive evaluations, treatment interventions, and patient education. The chosen duration directly impacts the per-session cost and influences the overall treatment timeline.
- Factors Influencing Duration:
Several factors influence the required session length, including the complexity of the condition, the patient’s current functional level, and the specific treatment goals. A patient recovering from a stroke, for example, might require longer sessions than someone managing a minor musculoskeletal injury. The therapist will assess these factors to determine the optimal session duration for maximizing therapeutic benefit.
- Cost Implications of Varying Durations:
Longer sessions generally incur higher costs due to the increased therapist time and resources allocated. While shorter sessions might appear more economical individually, they could necessitate more frequent visits to achieve the same therapeutic outcomes, potentially offsetting any initial cost savings. Balancing session duration with treatment frequency requires careful consideration of both therapeutic needs and budgetary constraints.
- Optimizing Session Time:
Maximizing the value of each session involves active patient participation and open communication with the therapist. Arriving prepared, asking clarifying questions, and diligently performing prescribed home exercises contribute to efficient use of session time and can optimize treatment outcomes. This proactive approach ensures patients receive the maximum benefit from each session, regardless of its duration.
By understanding the relationship between session duration, therapeutic needs, and cost, individuals can make informed decisions about their in-home physical therapy treatment plans. This awareness empowers patients to optimize their care while effectively managing financial resources, contributing to a positive and efficient rehabilitation journey.
3. Geographic Location
Geographic location significantly influences the cost of in-home physical therapy. Several factors related to location contribute to this variation, impacting affordability and access to care.
Cost of Living: Areas with higher costs of living generally experience higher healthcare expenses. This includes therapists’ operational costs, such as rent, utilities, and transportation, which are often passed on to patients. Metropolitan areas, for example, typically have higher session rates compared to rural regions due to increased overhead. This disparity reflects the economic realities of providing services in different geographic contexts.
Market Saturation and Competition: The number of therapists practicing in a given area influences pricing. Regions with a high concentration of providers may experience more competitive pricing due to increased supply. Conversely, areas with limited access to physical therapists may see higher rates due to decreased competition. Market dynamics play a crucial role in shaping the pricing landscape for in-home physical therapy services.
Travel Time and Expenses: Travel time represents a significant cost factor for therapists providing in-home care. In densely populated areas with heavy traffic, therapists may spend considerable time traveling between patients, potentially increasing their travel expenses. These factors can contribute to higher session rates, reflecting the time and resources required to reach patients in various locations. Rural areas, while potentially having lower overhead costs, may involve longer travel distances between patients, also influencing pricing.
Accessibility to Specialized Services: Access to specialized services can vary by location. Urban centers often have a greater concentration of therapists specializing in niche areas like pediatric neurology or sports rehabilitation. While this offers more choices for patients with specific needs, it can also lead to higher costs for specialized expertise. Patients in rural areas may face challenges accessing specialized care, potentially requiring travel to larger cities, adding to the overall expense.
Understanding the influence of geographic location on in-home physical therapy costs empowers patients to navigate the healthcare landscape effectively. Recognizing regional variations in pricing and service availability allows individuals to make informed decisions about accessing appropriate care within their budgetary constraints. This awareness promotes informed healthcare choices and ensures patients receive the most suitable care based on their specific needs and geographic context.
4. Specific Patient Needs
Individual patient needs directly influence the cost of in-home physical therapy. The complexity and severity of the condition, the required frequency and duration of treatment, and the need for specialized equipment or assistive devices all contribute to the overall expense. Understanding these factors empowers patients and caregivers to anticipate potential costs and make informed decisions regarding treatment plans.
- Type and Severity of Condition:
Conditions requiring specialized interventions, such as neurological rehabilitation following a stroke or complex orthopedic care after a joint replacement, often necessitate longer sessions, more specialized equipment, and potentially a higher frequency of visits. These factors contribute to increased costs compared to treating less complex conditions like a sprained ankle or general muscle weakness. The specific therapeutic approach and expertise required directly correlate with the overall expense.
- Required Frequency of Sessions:
Treatment frequency significantly impacts cost. Patients requiring multiple sessions per week, common in acute or complex cases, will incur higher expenses compared to those needing less frequent visits. The prescribed frequency depends on the individual’s condition, recovery progress, and overall treatment goals. Balancing therapeutic needs with financial constraints requires careful consideration of session frequency and its impact on the total cost.
- Need for Specialized Equipment:
Specialized equipment, such as ultrasound machines, electrical stimulation units, or therapeutic exercise devices, can add to the overall cost of in-home physical therapy. The need for such equipment depends on the specific condition and treatment plan. While some therapists may include equipment usage in their session fees, others may charge separately for equipment rental or purchase. Understanding these potential additional costs allows for better financial planning.
- Duration of Treatment:
The anticipated duration of treatment significantly impacts the total cost. Chronic conditions or complex injuries requiring extended rehabilitation periods will naturally incur higher expenses than short-term treatment for acute injuries. The projected treatment timeline, determined by the therapist’s assessment and the patient’s progress, influences the overall financial commitment required for successful rehabilitation.
By considering these factors, patients and caregivers gain a clearer understanding of how individual needs influence the cost of in-home physical therapy. This awareness facilitates informed decision-making, allowing individuals to balance their therapeutic requirements with budgetary considerations. Open communication with the therapist regarding treatment options and associated costs promotes a collaborative approach to care, ensuring patients receive effective and affordable rehabilitation services tailored to their specific circumstances.
5. Insurance Coverage
Insurance coverage plays a crucial role in managing the cost of in-home physical therapy. Policies vary significantly in terms of coverage for these services, influencing patient out-of-pocket expenses and access to care. Understanding insurance provisions is essential for navigating the financial aspects of in-home rehabilitation.
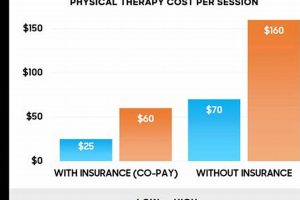
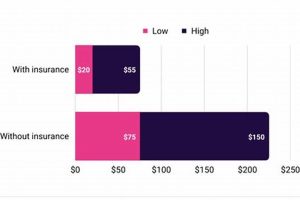
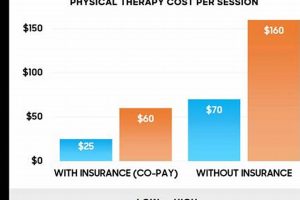
Several factors determine the extent of coverage. The specific insurance plan, the patient’s diagnosis, and the prescribed treatment plan all influence the level of reimbursement. Some plans may cover a percentage of the cost, while others might require a fixed co-pay per visit. Pre-authorization may be necessary before initiating treatment, ensuring the services align with the insurance company’s guidelines. For instance, a patient with a post-surgical rehabilitation plan might receive greater coverage than someone seeking treatment for a chronic condition. Furthermore, some plans may limit the number of covered visits within a specific timeframe. A clear understanding of these limitations enables proactive planning and informed decision-making.
Navigating insurance coverage requires proactive communication with both the insurance provider and the physical therapy clinic. Verifying coverage details, understanding pre-authorization requirements, and obtaining clear explanations of benefits are crucial steps. This proactive approach empowers patients to anticipate potential out-of-pocket expenses and make informed decisions about their treatment options. Failure to understand insurance provisions can lead to unexpected financial burdens, potentially delaying or hindering access to necessary rehabilitative care. Therefore, thorough understanding of insurance coverage is essential for managing the cost of in-home physical therapy effectively. This knowledge facilitates informed financial planning, ensures access to appropriate care, and ultimately contributes to a more positive and manageable rehabilitation experience.
6. Equipment Needs
Equipment needs significantly influence the overall cost of in-home physical therapy. While some therapeutic interventions rely primarily on the therapist’s expertise and patient engagement, others require specialized equipment to achieve optimal outcomes. Understanding these equipment needs and their associated costs allows for informed decision-making and effective budget management.
- Therapeutic Exercise Equipment:
Therapeutic exercise equipment, such as resistance bands, stability balls, and weights, can enhance in-home rehabilitation programs. These tools facilitate targeted exercises designed to improve strength, flexibility, and balance. Costs vary depending on the type and quality of equipment. While some items represent a relatively small investment, specialized exercise machines can incur substantial costs. Therapists often guide patients on appropriate equipment selection based on individual needs and budgetary considerations.
- Assistive Devices:
Individuals with mobility challenges may require assistive devices like walkers, canes, or crutches to enhance safety and independence during in-home therapy sessions. The cost of these devices varies depending on the specific type and features. Insurance coverage may offset some expenses, but patients often bear some financial responsibility for acquiring and maintaining these essential aids. Proper selection and fitting of assistive devices are crucial for maximizing their therapeutic benefit and ensuring patient safety.
- Electrotherapy Modalities:
Electrotherapy modalities, such as transcutaneous electrical nerve stimulation (TENS) units or ultrasound machines, are sometimes employed in in-home physical therapy to manage pain and promote tissue healing. These modalities often require specialized equipment that can contribute significantly to the overall cost of treatment. Therapists determine the appropriateness of electrotherapy based on individual patient needs and treatment goals. While these modalities can offer therapeutic benefits, their associated costs require careful consideration.
- Durable Medical Equipment (DME):
Durable medical equipment, such as wheelchairs, hospital beds, or patient lifts, might be necessary for individuals with significant functional limitations receiving in-home physical therapy. These items often represent substantial investments. Insurance coverage may vary, and patients frequently bear a portion of the financial burden. Careful assessment of DME needs and exploration of rental options can help manage expenses while ensuring access to essential equipment.
Careful consideration of equipment needs and associated costs is essential when planning for in-home physical therapy. Understanding the various types of equipment, their therapeutic benefits, and their potential impact on the overall budget empowers patients and caregivers to make informed decisions. Open communication with the therapist regarding equipment recommendations, rental options, and potential insurance coverage ensures cost-effective strategies for acquiring necessary tools to maximize therapeutic outcomes.
Frequently Asked Questions
This section addresses common inquiries regarding expenses associated with receiving physical therapy services in a residential setting. Clarity on these financial aspects empowers individuals to make informed healthcare decisions.
Question 1: How does one determine the average cost in a specific geographic area?
Consulting online resources that provide regional cost estimates for healthcare services or contacting local physical therapy clinics directly to inquire about pricing structures offers valuable insights.
Question 2: What factors influence the overall expense beyond the therapist’s hourly rate?
Factors such as the required duration of treatment, the need for specialized equipment, travel expenses for the therapist, and the complexity of the individual’s condition contribute to overall expenses.
Question 3: How does insurance typically handle coverage for these services?
Insurance coverage varies significantly depending on the specific policy. Contacting the insurance provider directly to verify coverage details and pre-authorization requirements is recommended.
Question 4: Are there strategies for minimizing out-of-pocket expenses?
Exploring options such as negotiating payment plans with the provider, inquiring about sliding-scale fees based on income, and maximizing the use of prescribed home exercise programs can potentially minimize out-of-pocket expenses.
Question 5: What are the potential long-term cost benefits of this approach?
Personalized in-home care can potentially reduce long-term healthcare costs by promoting faster recovery, preventing complications, and improving overall functional independence, potentially reducing the need for future medical interventions.
Question 6: How does one compare pricing among different providers effectively?
Requesting detailed cost breakdowns from multiple providers, considering factors beyond the hourly rate, such as experience, specialization, and included services, facilitates informed comparisons.
Understanding these aspects empowers individuals to navigate the financial landscape of in-home physical therapy effectively. Proactive planning and informed decision-making contribute to successful rehabilitation journeys.
The subsequent section offers a concluding perspective on the value of in-home physical therapy.
In-Home Physical Therapy Cost
Expenses associated with receiving physical therapy within the comfort of one’s home represent a significant investment in personal well-being. This exploration has delved into the multifaceted nature of these expenses, highlighting key factors such as therapist credentials, session duration, geographic location, individual patient needs, insurance coverage, and equipment requirements. Each element contributes uniquely to the overall cost, underscoring the importance of informed financial planning.
Effective management of these expenses requires proactive engagement and thorough consideration of available resources. Empowered by knowledge and a clear understanding of cost determinants, individuals can navigate the complexities of healthcare finances, ensuring access to valuable therapeutic interventions. Prudent financial planning, coupled with open communication between patients, therapists, and insurance providers, paves the way for successful rehabilitation journeys and improved long-term health outcomes. The potential benefits of personalized in-home care extend beyond immediate recovery, contributing to sustained well-being and enhanced quality of life.