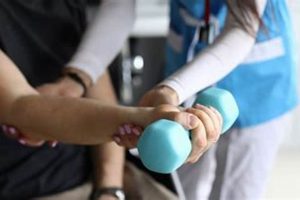
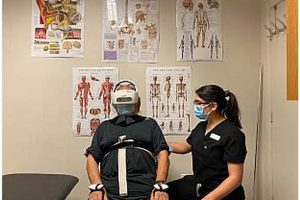
A specialized healthcare practice focuses on restoring movement, function, and overall well-being through evidence-based techniques. These techniques often include exercises, manual therapy, and modalities like ultrasound or electrical stimulation, tailored to address specific patient needs, such as recovering from injuries, managing chronic pain, or improving mobility limitations.
Restoring functional independence and improving quality of life are central to this practice. Through targeted interventions, patients can experience pain reduction, increased strength and flexibility, and improved cardiovascular health. The historical development of this field reflects an ongoing commitment to advancing patient care through research and innovation in treatment approaches.
Further exploration will delve into specific treatment modalities, the role of the therapist-patient relationship, and the integration of this practice within broader healthcare systems.
Tips for Optimizing Physical Well-being
Maximizing the benefits of therapeutic interventions requires active patient participation. The following recommendations offer practical strategies for improving outcomes and overall health.
Tip 1: Adherence to Prescribed Programs: Consistent engagement with prescribed exercises and activities is crucial for achieving therapeutic goals. Regular practice reinforces strength gains, promotes flexibility, and facilitates recovery.
Tip 2: Open Communication with Therapists: Clear and consistent communication with therapists regarding any discomfort or changes in condition allows for adjustments to treatment plans and ensures optimal progress.
Tip 3: Maintaining a Healthy Lifestyle: A balanced diet, adequate sleep, and stress management techniques complement therapeutic interventions, supporting overall well-being and maximizing recovery potential.
Tip 4: Gradual Progression of Activities: Respecting the body’s limitations and gradually increasing activity levels prevents setbacks and promotes long-term progress. Avoid pushing beyond comfortable limits, especially in the early stages of recovery.
Tip 5: Setting Realistic Expectations: Healing and recovery take time. Setting achievable goals and celebrating incremental progress fosters motivation and encourages long-term commitment to the therapeutic process.
Tip 6: Active Participation in Home Exercise Programs: Consistent completion of prescribed home exercises reinforces gains made during therapy sessions and accelerates progress toward recovery.
Tip 7: Integrating Therapeutic Principles into Daily Life: Applying learned techniques, such as proper posture and body mechanics, to everyday activities promotes long-term health and prevents recurrence of issues.
By integrating these recommendations, individuals can optimize the benefits of therapy, improve overall well-being, and achieve lasting improvements in physical function.
The strategies outlined above provide a foundation for a proactive approach to health management and long-term wellness. Further sections will explore specific treatment modalities and the importance of individualized care plans.
1. Personalized Treatment Plans
Personalized treatment plans constitute a cornerstone of effective physical therapy practice. Individualized approaches recognize that each patient presents with unique circumstances, including specific injuries, medical histories, and personal goals. A tailored plan considers these factors to optimize treatment effectiveness and ensure alignment with individual needs. This approach contrasts with standardized protocols, offering a more precise and effective path toward recovery. For instance, a patient recovering from a stroke will require a different rehabilitation strategy than an athlete recovering from a torn ligament, even if some underlying therapeutic principles overlap. The personalized approach allows practitioners to select the most appropriate techniques and exercises, maximizing the potential for positive outcomes.
The process of developing a personalized treatment plan often involves a thorough initial assessment to determine the patient’s current physical condition, functional limitations, and specific goals. This assessment may include evaluating range of motion, strength, balance, and pain levels. The therapist then collaborates with the patient to establish realistic and achievable goals, outlining the specific interventions to be employed, the anticipated timeframe for progress, and the expected outcomes. Ongoing monitoring and adjustments to the plan are essential to accommodate the patient’s evolving needs and ensure continued progress. This dynamic approach ensures the plan remains relevant and effective throughout the recovery process. For example, a patient initially focused on pain management may transition to exercises designed to improve strength and mobility as their condition improves.
The emphasis on personalized treatment plans reflects a commitment to patient-centered care. Recognizing individual needs and tailoring treatment accordingly maximizes the likelihood of successful outcomes and fosters a collaborative relationship between patient and therapist. This approach underscores the importance of considering the whole person, rather than solely focusing on the specific injury or condition. By addressing the individual’s unique circumstances and goals, physical therapy can effectively promote improved function, reduced pain, and enhanced quality of life.
2. Evidence-Based Techniques
Effective physical therapy relies on evidence-based techniques, integrating the best available research with clinical expertise and patient values. This approach ensures treatments are safe, effective, and tailored to individual needs, reflecting a commitment to continuous improvement and optimal patient outcomes within the context of physical therapy practice. Prioritizing evidence-based practices fosters confidence in the chosen interventions and maximizes the potential for successful rehabilitation.
- Systematic Reviews and Meta-Analyses
Systematic reviews and meta-analyses synthesize data from multiple studies, providing a comprehensive overview of the effectiveness of specific interventions. For example, a review might analyze the effectiveness of different exercise protocols for patients recovering from rotator cuff injuries. These analyses inform clinical decision-making, ensuring treatments align with the most current scientific understanding. This rigorous approach allows practitioners to select interventions with proven efficacy, maximizing the potential for positive patient outcomes.
- Randomized Controlled Trials (RCTs)
RCTs are considered the gold standard for evaluating treatment effectiveness. These studies randomly assign participants to different treatment groups, allowing researchers to isolate the effects of a specific intervention. For instance, an RCT might compare the effectiveness of manual therapy versus therapeutic exercise in managing low back pain. The rigorous design of RCTs minimizes bias and provides strong evidence regarding the efficacy of different treatments. The results of RCTs directly inform clinical practice, guiding the selection of interventions most likely to produce favorable results.
- Clinical Practice Guidelines
Clinical practice guidelines translate research findings into practical recommendations for practitioners. These guidelines provide evidence-based algorithms for managing specific conditions, offering standardized approaches to care. For example, guidelines for managing osteoarthritis might recommend a combination of exercise, manual therapy, and patient education. Adherence to clinical practice guidelines ensures consistent delivery of high-quality care, promoting optimal patient outcomes and reducing variations in practice. These guidelines offer a valuable framework for practitioners, ensuring treatments align with current best practices.
- Outcome Measures
Outcome measures quantify patient progress and evaluate the effectiveness of interventions. These measures can include assessments of pain, range of motion, functional capacity, and quality of life. Tracking outcome measures allows practitioners to monitor patient response to treatment and make necessary adjustments to the plan of care. For instance, regular assessment of pain levels can help determine whether a particular intervention is effectively alleviating discomfort. Utilizing outcome measures ensures accountability and provides valuable data for continuous improvement of treatment protocols. This data-driven approach allows practitioners to refine their techniques and optimize patient outcomes.
These facets of evidence-based practice demonstrate a commitment to providing the most effective and up-to-date care within physical therapy. By integrating research findings, clinical expertise, and patient preferences, physical therapy practitioners strive to optimize patient outcomes, enhance quality of life, and promote long-term well-being. This dedication to evidence-based care distinguishes effective physical therapy practices and ensures patients receive the highest standard of care.
3. Manual Therapy
Manual therapy represents a cornerstone of many effective physical therapy practices, encompassing a range of hands-on techniques used to diagnose and treat musculoskeletal dysfunction. These techniques address impairments in joints, muscles, and connective tissues, aiming to reduce pain, improve range of motion, and restore optimal function. Within a comprehensive physical therapy program, manual therapy frequently complements other interventions, such as therapeutic exercise and modalities, creating a synergistic approach to patient care. The integration of manual therapy can be particularly beneficial in addressing conditions like back pain, neck pain, and joint stiffness. For example, mobilization techniques can restore joint mobility in patients experiencing limitations due to osteoarthritis, while soft tissue mobilization can address muscle tension and trigger points contributing to headaches or back pain. The skilled application of manual therapy techniques plays a significant role in facilitating recovery and improving overall patient outcomes.
The efficacy of manual therapy stems from its ability to directly address the underlying causes of musculoskeletal dysfunction. By restoring proper joint mechanics, reducing muscle tension, and improving tissue mobility, manual therapy creates a physiological environment conducive to healing and improved function. For instance, in a patient with a restricted shoulder joint following surgery, manual therapy techniques can improve joint mobility, allowing for a greater range of motion during therapeutic exercises. This combined approach maximizes the benefits of exercise and accelerates the recovery process. Furthermore, manual therapy can facilitate improved neuromuscular control, enhancing the patient’s ability to activate and coordinate muscle activity. This improved control contributes to enhanced stability, reduced risk of re-injury, and improved long-term functional outcomes.
The integration of manual therapy within a comprehensive physical therapy program offers significant benefits for patients seeking to restore function, reduce pain, and improve overall well-being. Through skilled application of hands-on techniques, therapists can address musculoskeletal impairments, promote tissue healing, and facilitate optimal movement patterns. The resulting improvements in joint mobility, muscle function, and neuromuscular control contribute to enhanced physical function, improved quality of life, and reduced risk of future injury. While manual therapy represents a valuable component of many successful physical therapy programs, its important to acknowledge that its effectiveness often relies on the skill and expertise of the treating therapist, accurate diagnosis, and appropriate integration with other therapeutic interventions.
4. Therapeutic Exercise
Therapeutic exercise forms an integral component of effective physical therapy interventions, serving as a cornerstone of programs aimed at restoring function, improving mobility, and alleviating pain. Within the context of a comprehensive approach like that often employed in practices such as Hughes Physical Therapy, therapeutic exercise plays a crucial role in achieving patient-centered goals. This connection stems from the fundamental principle that controlled movement, guided by expert knowledge and tailored to individual needs, is essential for healing and functional recovery. The specific exercises prescribed are determined by a thorough assessment of the patient’s condition, taking into account factors such as injury type, pain levels, range of motion limitations, and overall functional capacity. For instance, a patient recovering from a knee injury might engage in exercises designed to strengthen the surrounding musculature, improve joint stability, and restore normal gait patterns, while a patient managing chronic back pain might focus on exercises that improve core strength, flexibility, and postural control. This individualized approach ensures that therapeutic exercise addresses the unique needs of each patient, maximizing the potential for positive outcomes.
The practical significance of understanding the connection between therapeutic exercise and comprehensive physical therapy programs lies in its impact on patient recovery and long-term well-being. Therapeutic exercise not only addresses the immediate symptoms of a condition but also empowers patients to actively participate in their own recovery. By engaging in prescribed exercises, patients gain a sense of control over their rehabilitation process and develop strategies for managing their condition independently. This active participation fosters adherence to treatment plans and promotes long-term health benefits. Real-life examples abound. Athletes recovering from sports injuries utilize therapeutic exercise to regain strength, flexibility, and sport-specific skills, while individuals managing chronic conditions like arthritis use exercise to maintain joint mobility, reduce pain, and improve overall quality of life. Furthermore, therapeutic exercise can play a crucial role in preventing future injuries by strengthening supporting muscles, improving balance, and promoting proper movement patterns. These preventive benefits highlight the long-term value of integrating therapeutic exercise into a comprehensive physical therapy plan.
In summary, therapeutic exercise serves as a critical component within the framework of comprehensive physical therapy practices, such as those exemplified by Hughes Physical Therapy. The individualized nature of prescribed exercises ensures that interventions address specific patient needs, promoting optimal recovery and functional restoration. By actively participating in therapeutic exercise, patients become empowered in their healing journey, gaining control over their condition and developing strategies for long-term well-being. The practical application of this understanding results in improved outcomes, enhanced quality of life, and reduced risk of future injury, underscoring the essential role of therapeutic exercise in achieving optimal physical health.
5. Pain Management
Effective pain management constitutes a critical component of physical therapy practice, significantly influencing patient outcomes and overall well-being. Within the context of a comprehensive approach, such as that often seen in practices like Hughes Physical Therapy, pain management strategies are integrated into personalized treatment plans, addressing both the underlying causes and the symptomatic manifestations of pain. This integrated approach recognizes the multifaceted nature of pain, acknowledging its physiological, psychological, and social dimensions. Effective pain management not only alleviates discomfort but also facilitates engagement in therapeutic exercises and activities, promoting functional recovery and improving quality of life. The following facets explore key components of pain management within the broader framework of physical therapy.
- Manual Therapy Techniques
Manual therapy techniques, including joint mobilization, soft tissue mobilization, and myofascial release, can directly address musculoskeletal impairments contributing to pain. By restoring proper joint mechanics, reducing muscle tension, and improving tissue mobility, manual therapy can alleviate discomfort and improve function. For example, a patient experiencing back pain due to muscle spasms might benefit from soft tissue mobilization to release tension and reduce pain, allowing for increased participation in therapeutic exercise. The hands-on nature of these techniques allows therapists to precisely target areas of dysfunction, providing effective pain relief and facilitating progress toward functional goals. The integration of manual therapy techniques within a comprehensive pain management plan highlights the importance of addressing the underlying musculoskeletal contributors to pain.
- Therapeutic Modalities
Therapeutic modalities, such as ultrasound, electrical stimulation, and heat/ice therapy, can provide effective pain relief and promote tissue healing. Ultrasound can reduce inflammation and promote tissue repair, while electrical stimulation can modulate pain signals and improve muscle function. Heat therapy can relax muscles and increase blood flow, while ice therapy can reduce inflammation and numb pain. A patient experiencing acute pain following an ankle sprain might benefit from ice therapy to reduce swelling and pain, followed by ultrasound to promote tissue healing. The judicious application of therapeutic modalities, tailored to the specific needs of each patient, enhances pain management and facilitates progress within a comprehensive physical therapy program.
- Therapeutic Exercise
Therapeutic exercise plays a crucial role in managing pain by strengthening muscles, improving joint stability, and restoring optimal movement patterns. Targeted exercises can address specific impairments contributing to pain, such as muscle weakness, joint instability, or poor posture. A patient with chronic knee pain might benefit from exercises designed to strengthen the quadriceps and hamstring muscles, improving joint stability and reducing pain. Furthermore, exercise releases endorphins, which have natural pain-relieving effects. By promoting physical function and reducing reliance on pain medication, therapeutic exercise contributes to long-term pain management and improved quality of life.
- Patient Education
Educating patients about their condition, pain mechanisms, and self-management strategies empowers them to actively participate in their pain management plan. Understanding the nature of their pain can reduce anxiety and improve coping mechanisms. Providing patients with practical strategies for managing pain, such as pacing activities, using proper body mechanics, and incorporating stress management techniques, can significantly enhance their ability to control their pain and improve overall function. For instance, a patient with chronic low back pain might benefit from education on proper lifting techniques and ergonomic modifications to reduce strain on the back and minimize pain flare-ups. Empowering patients through education promotes self-efficacy and fosters a collaborative approach to pain management.
These integrated facets of pain management within a comprehensive physical therapy program, as often implemented within practices like Hughes Physical Therapy, underscore a commitment to addressing the multifaceted nature of pain. By combining manual therapy, therapeutic modalities, therapeutic exercise, and patient education, physical therapists provide effective pain relief, facilitate functional restoration, and empower patients to actively participate in their recovery. This holistic approach recognizes that successful pain management is not simply about alleviating symptoms but also about addressing the underlying causes of pain and equipping patients with the tools and knowledge to manage their condition effectively, ultimately improving their overall quality of life.
6. Injury Rehabilitation
Injury rehabilitation represents a core focus within physical therapy practice, aiming to restore function, reduce pain, and facilitate a safe return to activity following injury. Within frameworks like those potentially employed at Hughes Physical Therapy, injury rehabilitation programs are individualized, addressing the specific needs of each patient and the unique demands of their respective injuries. These programs often integrate various therapeutic interventions, including manual therapy, therapeutic exercise, and modalities, to optimize recovery and prevent re-injury. The following facets delve into key components of effective injury rehabilitation programs.
- Comprehensive Assessment and Diagnosis
A thorough assessment forms the foundation of any successful injury rehabilitation program. This process involves evaluating the nature and extent of the injury, identifying contributing factors, and establishing baseline measurements of strength, range of motion, and functional capacity. Accurate diagnosis is essential for developing a targeted treatment plan. For example, a comprehensive assessment of a knee injury might involve evaluating ligament stability, assessing muscle strength imbalances, and analyzing movement patterns to identify biomechanical deficits. This information informs the development of a personalized rehabilitation program tailored to the specific needs of the patient.
- Individualized Treatment Plans
Injury rehabilitation programs are individualized, taking into account the specific needs of each patient and the unique demands of their injury. Treatment plans outline specific goals, therapeutic interventions, and anticipated timelines for recovery. For instance, a rehabilitation program for a shoulder injury might include exercises to improve range of motion, strengthen rotator cuff muscles, and restore functional stability. The individualized approach ensures the program addresses the specific impairments and functional limitations resulting from the injury, maximizing the potential for a full recovery.
- Progressive Exercise Progression
Therapeutic exercise plays a central role in injury rehabilitation, promoting tissue healing, restoring strength and flexibility, and improving functional capacity. Exercises are progressively advanced as the patient heals, gradually increasing the demands placed on the injured tissues. For example, a patient recovering from an ankle sprain might initially perform range of motion exercises, progressing to weight-bearing exercises and eventually plyometric activities as the injury heals. This progressive approach ensures tissues are challenged appropriately, promoting optimal recovery and minimizing the risk of re-injury.
- Functional Restoration and Return to Activity
The ultimate goal of injury rehabilitation is to restore functional capacity and facilitate a safe return to pre-injury activity levels. This involves incorporating functional exercises that mimic real-life movements and activities. For example, an athlete recovering from a hamstring injury might engage in sport-specific drills to regain agility, speed, and power. The focus on functional restoration ensures the rehabilitation program translates to improved performance in everyday activities and reduces the risk of future injury. The criteria for returning to activity are individualized, considering factors such as pain levels, functional capacity, and the demands of the activity.
These facets collectively illustrate a patient-centered approach to injury rehabilitation, emphasizing individualized care, progressive exercise progression, and functional restoration. Within a framework like that potentially employed at Hughes Physical Therapy, these principles guide the development and implementation of effective rehabilitation programs, facilitating safe and optimal recovery following injury.
7. Improved Mobility
Improved mobility stands as a central objective within physical therapy, representing a significant marker of progress and a key contributor to enhanced quality of life. Within the context of a practice like Hughes Physical Therapy, restoring and enhancing mobility serves as a cornerstone of treatment plans, impacting patient outcomes and long-term well-being. Mobility encompasses not only the ability to move freely and easily but also the capacity to engage in daily activities without restriction or pain. The following facets explore key components of improved mobility within the broader framework of physical therapy.
- Range of Motion Restoration
Restoring optimal range of motion in affected joints forms a foundational element of improved mobility. Limitations in range of motion can significantly impair function, restricting participation in daily activities and contributing to pain. Physical therapy interventions, such as manual therapy techniques and targeted exercises, address joint restrictions, promoting improved flexibility and mobility. For instance, a patient recovering from a shoulder injury might engage in range of motion exercises and receive manual therapy to restore full shoulder mobility, facilitating activities like reaching overhead or dressing independently. Restoring range of motion not only improves physical function but also reduces pain and enhances overall quality of life.
- Strength and Muscle Function Enhancement
Adequate muscle strength and optimal muscle function are essential for supporting movement and maintaining stability. Weakness or imbalances in muscle groups can compromise mobility and increase the risk of injury. Therapeutic exercises play a crucial role in strengthening key muscle groups, improving neuromuscular control, and enhancing overall movement efficiency. For example, a patient with knee osteoarthritis might engage in exercises to strengthen quadriceps and hamstring muscles, improving knee stability and facilitating activities like walking and stair climbing. Strengthening exercises not only improve mobility but also reduce pain and enhance functional independence.
- Balance and Coordination Improvement
Balance and coordination are integral components of mobility, influencing the ability to maintain postural control and execute smooth, controlled movements. Impairments in balance and coordination can increase the risk of falls and limit participation in various activities. Physical therapy interventions, including balance training exercises and proprioceptive training, enhance postural stability and improve neuromuscular control, promoting safer and more efficient movement. For example, an older adult seeking to improve balance might participate in exercises that challenge postural stability, improving their ability to navigate uneven surfaces and reducing their risk of falls. Improving balance and coordination enhances mobility, promotes independence, and reduces the risk of injury.
- Functional Mobility Enhancement
The ultimate goal of improved mobility within physical therapy is to enhance functional capacity, enabling individuals to engage in meaningful activities without restriction. Functional mobility encompasses the ability to perform tasks essential for daily living, such as walking, dressing, and transferring. Physical therapy programs incorporate functional exercises and activities that replicate real-life movements, promoting improved performance and independence. For example, a patient recovering from a stroke might engage in tasks like reaching, grasping, and walking to improve their ability to perform daily activities. The focus on functional mobility ensures that improvements in range of motion, strength, and balance translate to meaningful gains in everyday life.
These facets collectively highlight the multifaceted nature of improved mobility within the context of physical therapy. By addressing range of motion limitations, enhancing strength and muscle function, improving balance and coordination, and focusing on functional mobility, physical therapy interventions promote independence, reduce pain, and enhance overall quality of life. Within a practice like Hughes Physical Therapy, these principles likely underpin treatment approaches, guiding patients towards achieving their mobility goals and optimizing their long-term well-being. The emphasis on improved mobility reflects a commitment to restoring not only physical function but also the ability to live a full and active life.
Frequently Asked Questions
This section addresses common inquiries regarding physical therapy, providing concise and informative responses.
Question 1: What conditions can benefit from physical therapy?
Numerous conditions, including musculoskeletal injuries, neurological disorders, chronic pain syndromes, and post-surgical rehabilitation, can benefit. Specific examples include back pain, arthritis, stroke recovery, and sports injuries. A thorough assessment determines the appropriateness of therapy for individual circumstances.
Question 2: How long does a typical physical therapy session last?
Session duration varies depending on individual needs and treatment plans. Typically, sessions range from 30 to 60 minutes, potentially extending to 90 minutes for complex cases. The treating therapist determines the appropriate duration based on the patient’s specific requirements.
Question 3: What should one wear to a physical therapy appointment?
Comfortable, loose-fitting clothing that allows for free movement is recommended. Athletic wear or comfortable casual attire is generally appropriate. Patients should avoid restrictive clothing that may impede movement during assessment and treatment.
Question 4: What is the difference between physical therapy and chiropractic care?
While both professions address musculoskeletal issues, their approaches differ. Physical therapy emphasizes restoring function and mobility through exercise, manual therapy, and other modalities. Chiropractic care focuses primarily on spinal manipulation to address joint alignment and nerve function. Both professions can play valuable roles in managing musculoskeletal conditions.
Question 5: Is physical therapy painful?
Some discomfort may be experienced during certain treatments, particularly when addressing areas of injury or inflammation. Therapists prioritize patient comfort and adjust treatment intensity as needed. Open communication between patient and therapist is crucial for managing discomfort and ensuring a positive treatment experience. While some therapeutic techniques may involve temporary discomfort, the goal is to reduce pain and improve function over time.
Question 6: How frequently are physical therapy appointments necessary?
Appointment frequency depends on individual needs and the nature of the condition being addressed. Initially, more frequent sessions may be recommended to establish a foundation for recovery. As progress is made, the frequency may decrease. The treating therapist determines the optimal frequency based on the patient’s specific circumstances and progress towards goals.
Understanding the answers to these common questions facilitates informed decision-making and promotes a positive experience within physical therapy.
Further sections will explore specific treatment modalities and their respective benefits within a comprehensive physical therapy program.
Conclusion
This exploration of specialized physical therapy, potentially exemplified by a practice like Hughes Physical Therapy, has highlighted the multifaceted nature of restoring movement, function, and overall well-being. Key aspects discussed include the importance of personalized treatment plans, the integration of evidence-based techniques, the role of manual therapy and therapeutic exercise, and the focus on effective pain management and injury rehabilitation. The significance of improved mobility as a central objective has also been underscored, emphasizing its impact on patient outcomes and quality of life.
Achieving optimal physical health requires a proactive and informed approach. Individuals experiencing pain, limited mobility, or other functional limitations are encouraged to seek professional guidance. Effective physical therapy interventions offer a pathway toward improved well-being, empowering individuals to regain control over their physical health and enhance their quality of life. Continued advancements in the field promise further refinements in treatment approaches and expanded opportunities for individuals seeking optimal physical function and overall well-being.