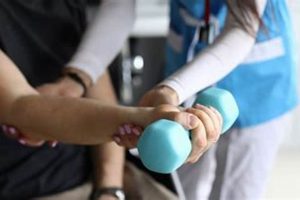
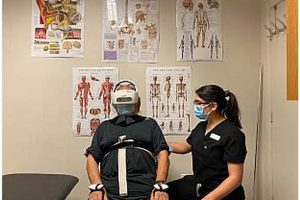
Securing additional sessions of rehabilitative care under existing insurance coverage often involves a multifaceted approach. This can include demonstrating medical necessity through detailed documentation of ongoing functional limitations and progress, open communication with the prescribing physician regarding treatment goals and efficacy, and appeals processes if initial requests are denied. For example, a patient might require extended care for a complex injury requiring a longer recovery period than initially anticipated. In such cases, providing comprehensive documentation of slow but steady progress is crucial.
Maximizing insurance benefits for rehabilitation services is essential for optimizing patient recovery and functional outcomes. Adequate treatment duration facilitates comprehensive rehabilitation, minimizing the risk of re-injury and chronic pain. Historically, access to these services has been influenced by evolving insurance policies and healthcare regulations. Understanding these changes empowers patients to advocate for their healthcare needs effectively.
Several key strategies can assist individuals in navigating the process of obtaining necessary rehabilitation services. These include understanding policy limitations, effectively communicating with healthcare providers, and exploring available appeals options when applicable. The following sections will delve into each of these areas in greater detail.
Tips for Obtaining Necessary Rehabilitation Services
Obtaining appropriate coverage for rehabilitative care requires proactive engagement with the healthcare system. The following tips provide guidance on navigating this process effectively.
Tip 1: Thorough Documentation: Maintain comprehensive records of all therapy sessions, including progress notes, treatment plans, and any relevant test results. Detailed documentation strengthens the case for medical necessity when requesting additional sessions.
Tip 2: Open Communication with the Prescribing Physician: Regular communication with the prescribing physician is crucial. Ensure the physician is aware of ongoing functional limitations and the impact on daily activities. Physician advocacy plays a significant role in justifying extended care.
Tip 3: Understand Policy Limitations: Carefully review insurance policy documents to understand coverage limitations for physical therapy services. This knowledge informs realistic expectations and facilitates proactive planning.
Tip 4: Pre-Authorization: Contact the insurance provider to determine if pre-authorization is required for additional visits. Initiating this process early can prevent delays in treatment.
Tip 5: Appeals Process: If initial requests for additional visits are denied, understand the appeals process. Gather supporting documentation and clearly articulate the rationale for continued care in the appeal.
Tip 6: Explore Alternative Treatment Options: If insurance coverage limitations pose challenges, explore alternative treatment options, such as home exercise programs or group therapy sessions, which may be more cost-effective.
Tip 7: Consult with a Case Manager: Many insurance providers offer case management services. A case manager can provide guidance on navigating the system and maximizing available benefits.
By actively participating in the process and understanding available resources, individuals can significantly improve their chances of obtaining the necessary rehabilitation services to achieve optimal functional recovery.
Through proactive engagement and informed decision-making, individuals can navigate the complexities of insurance coverage and secure the necessary support for their rehabilitation journey.
1. Medical Necessity
Medical necessity forms the cornerstone of securing additional physical therapy visits under insurance coverage. It signifies that the requested treatment is essential for restoring functional capacity and addressing a specific medical condition, not merely for convenience or general wellness. Insurance providers require demonstrable evidence of this need, linking the requested therapy to a diagnosed condition and its impact on the patient’s ability to perform daily activities. For example, a patient recovering from a stroke might require extended physical therapy to regain lost motor skills crucial for independent living. Without establishing this connection, requests for additional visits are likely to be denied.
Establishing medical necessity requires detailed documentation, including the initial diagnosis, treatment plan, progress notes, and objective measures of functional improvement. This documentation should clearly articulate how continued therapy directly addresses the identified impairments and contributes to measurable functional gains. Furthermore, the documentation must demonstrate that the prescribed therapy is the most appropriate and cost-effective intervention for the specific condition. For instance, documentation might illustrate how continued physical therapy sessions directly improve a patient’s range of motion, strength, and balance, ultimately enabling them to perform essential daily tasks, such as dressing or walking independently. Such concrete examples strengthen the case for medical necessity.
Understanding the concept of medical necessity and its practical application is paramount for patients seeking extended physical therapy coverage. By working closely with healthcare providers to ensure comprehensive documentation and a clear articulation of the need for continued care, patients can significantly improve their chances of securing the necessary support for optimal recovery. Failure to effectively establish medical necessity often results in denied claims and potentially compromised rehabilitation outcomes. Therefore, proactive communication and meticulous record-keeping are essential for navigating the complexities of insurance coverage and achieving desired functional goals.
2. Physician Advocacy
Physician advocacy plays a pivotal role in securing necessary physical therapy services under insurance coverage. Insurance providers often rely on the expertise and judgment of the prescribing physician to determine the appropriateness and medical necessity of extended care. A strong advocate can effectively articulate the patient’s needs, connecting ongoing functional limitations to the diagnosed condition and demonstrating how continued therapy contributes to measurable improvements. This advocacy goes beyond simply prescribing therapy; it involves actively communicating with the insurance provider, providing detailed documentation supporting the request, and addressing any concerns or questions raised by the insurer. For example, a physician might provide specific examples of how a patient’s limited range of motion in their shoulder, resulting from a rotator cuff injury, impacts their ability to perform essential job functions, justifying the need for additional physical therapy sessions to restore full functionality and prevent long-term disability. Without strong physician support, requests for additional visits are less likely to be approved.
The effectiveness of physician advocacy stems from their understanding of both the patient’s medical condition and the nuances of insurance requirements. They can translate complex medical information into clear, concise justifications for continued care, highlighting the specific benefits of extended therapy and the potential negative consequences of premature discontinuation. This expertise lends credibility to the request and strengthens the case for medical necessity. In cases involving complex or chronic conditions, physician advocacy becomes even more critical. They can provide a comprehensive overview of the patient’s medical history, treatment progress, and future rehabilitation needs, painting a clear picture of the long-term benefits of continued physical therapy. This proactive approach can preempt potential denials and ensure the patient receives the necessary support for optimal recovery. For example, if a patient with multiple sclerosis experiences a relapse affecting their mobility, the physician can detail how physical therapy can help manage symptoms, improve function, and prevent further decline, supporting the request for additional sessions.
Securing adequate physical therapy coverage often depends on the strength of physician advocacy. Patients benefit significantly when their physicians actively champion their need for continued care. This advocacy not only increases the likelihood of approval for additional visits but also empowers patients in the process, ensuring their voices are heard and their healthcare needs are met. Challenges may arise when communication between the physician’s office and the insurance provider is inefficient or when documentation lacks sufficient detail. Addressing these potential roadblocks through proactive communication and comprehensive record-keeping strengthens the overall case for extended care and facilitates a smoother process for all parties involved. Ultimately, effective physician advocacy is essential for optimizing patient outcomes and ensuring access to the necessary resources for successful rehabilitation.
3. Clear Documentation
Clear documentation provides a demonstrable foundation for justifying extended physical therapy services under insurance coverage. It serves as objective evidence of medical necessity, linking the requested treatment to a diagnosed condition, outlining the treatment plan, and tracking progress toward functional goals. Meticulous record-keeping strengthens the case for additional visits by providing concrete examples of how continued therapy directly addresses specific impairments and contributes to measurable improvements. For instance, documentation detailing a patient’s limited range of motion following a knee surgery, alongside progress notes showing gradual improvement through prescribed exercises, substantiates the need for continued physical therapy to achieve full functional recovery. Without such clear documentation, requests for additional visits may lack the necessary support and are more likely to be denied. The cause-and-effect relationship is clear: comprehensive documentation increases the probability of securing necessary care.
Comprehensive documentation comprises several key elements: a clear diagnosis, a detailed treatment plan outlining specific therapeutic interventions, progress notes documenting each session’s activities and the patient’s response, and objective measures of functional improvement, such as range of motion, strength, and pain levels. This comprehensive approach provides a holistic view of the patient’s progress, demonstrating the efficacy of the prescribed therapy and justifying the need for continued care. For example, a patient recovering from a shoulder injury might have documentation showing initial limitations in lifting their arm, followed by progressive improvements in strength and range of motion over subsequent therapy sessions, demonstrating the value of continued treatment. This data-driven approach strengthens the argument for extended care, presenting a compelling case to insurance providers. Furthermore, clear documentation facilitates communication between the treating therapist, the prescribing physician, and the insurance provider, ensuring all parties are informed of the patient’s progress and the rationale for continued care.
Understanding the importance of clear documentation empowers patients to actively participate in their rehabilitation journey. By working closely with their healthcare providers to ensure comprehensive and accurate record-keeping, patients can significantly influence the outcome of requests for extended care. This proactive approach not only increases the likelihood of approval but also fosters a sense of collaboration and shared decision-making between the patient and the healthcare team. Challenges can arise when documentation is incomplete, inconsistent, or lacks specific, measurable outcomes. Addressing these challenges through standardized documentation practices and regular communication between healthcare providers and patients strengthens the overall case for extended care and ensures optimal utilization of insurance benefits. Ultimately, clear documentation serves as a cornerstone of effective advocacy for necessary physical therapy services, optimizing patient outcomes and promoting efficient utilization of healthcare resources.
4. Understanding Policy
Navigating insurance policies effectively is crucial for securing necessary physical therapy services. Policy limitations, pre-authorization requirements, and appeals processes directly influence the accessibility of extended care. A thorough understanding of these aspects empowers individuals to advocate for their healthcare needs and maximize available benefits. Policy comprehension allows for proactive planning and informed decision-making, ultimately impacting the duration and scope of covered physical therapy services.
- Coverage Limitations
Policies often specify the number of physical therapy visits allowed within a given timeframe or for a specific condition. Understanding these limitations is essential for setting realistic expectations and exploring alternative options if the initial authorization proves insufficient. For instance, a policy might cover 20 visits per year for a specific diagnosis. Exceeding this limit requires pre-authorization or appeals, supported by robust medical necessity documentation. Ignoring these limitations can lead to unexpected out-of-pocket expenses.
- Pre-Authorization Requirements
Many insurance plans require pre-authorization for certain medical procedures, including extended physical therapy services. This process involves obtaining approval from the insurance provider before commencing treatment beyond the initially authorized scope. Pre-authorization necessitates timely communication with the provider and the submission of supporting documentation outlining the medical necessity of additional visits. Failing to obtain pre-authorization can result in denied claims and financial responsibility for the uncovered services. For example, a patient requiring specialized therapy beyond the initially authorized sessions might need pre-authorization, emphasizing the importance of proactive communication with the insurance provider and the prescribing physician. Understanding pre-authorization procedures is crucial for a smooth continuation of care.
- Appeals Processes
When requests for additional physical therapy visits are denied, a formal appeals process allows individuals to challenge the decision. Understanding this process, including deadlines, required documentation, and the levels of appeal, is critical for advocating effectively for continued care. A successful appeal often hinges on presenting a compelling case supported by strong medical necessity documentation, physician advocacy, and a clear articulation of the benefits of extended therapy. Navigating the appeals process effectively requires persistence, organization, and a clear understanding of the insurance policy’s provisions regarding dispute resolution. For example, if a claim is denied due to insufficient documentation, a well-crafted appeal incorporating additional medical records and a strong letter of support from the physician can reverse the decision.
- Exclusions and Inclusions
Insurance policies explicitly state covered and excluded services. Thoroughly reviewing these details clarifies which types of physical therapy modalities, such as manual therapy or aquatic therapy, are covered under the policy and under what conditions. Understanding these inclusions and exclusions is crucial for making informed decisions about treatment options and avoiding unexpected costs. For example, a policy might cover standard physical therapy but exclude specialized treatments like vestibular rehabilitation. Understanding these nuances ensures realistic expectations and facilitates informed decision-making regarding alternative therapies or out-of-pocket expenses. This knowledge empowers individuals to explore all available options within their coverage and advocate for medically necessary services.
By understanding the nuances of insurance policies, individuals can effectively navigate the complexities of the healthcare system, maximize available benefits, and secure the necessary physical therapy services to achieve optimal recovery. This proactive approach not only empowers patients in their healthcare journey but also facilitates efficient utilization of healthcare resources and promotes positive treatment outcomes. Failure to grasp these key policy aspects can lead to denied claims, unexpected financial burdens, and potentially compromised rehabilitation progress. Therefore, investing time and effort in understanding policy details is a critical step toward successful management of physical therapy needs.
5. Appeals Processes
Appeals processes represent a critical pathway for securing additional physical therapy visits when initial requests are denied by insurance providers. Denials often stem from discrepancies between requested services and perceived medical necessity as defined by the insurer’s criteria. A robust appeals process provides a mechanism for challenging these denials, offering an opportunity to present a more comprehensive picture of the individual’s functional limitations, treatment progress, and the potential benefits of extended care. This process underscores the importance of thorough documentation, clear communication between healthcare providers and the insurer, and a comprehensive understanding of the policy’s provisions regarding appeals. For example, if initial authorization for post-surgical rehabilitation is limited to a specific number of sessions deemed insufficient by the treating physician, the appeals process allows for the submission of additional documentation, such as progress notes demonstrating slower-than-expected recovery or persistent functional deficits, along with a letter of medical necessity from the physician, advocating for extended care. Without access to a structured appeals process, individuals face limited recourse for obtaining medically necessary services beyond the initial authorization, potentially jeopardizing optimal recovery.
Effectively navigating the appeals process requires a strategic approach, emphasizing clear, concise communication and compelling evidence supporting the need for extended care. This involves gathering all relevant medical records, including diagnostic reports, treatment plans, progress notes, and any objective measures of functional improvement. A well-crafted appeal letter should clearly articulate the rationale for continued physical therapy, linking ongoing functional limitations to the diagnosed condition and demonstrating how additional sessions directly contribute to measurable progress toward recovery goals. Supporting documentation from the prescribing physician, emphasizing medical necessity and outlining the potential negative consequences of prematurely discontinuing therapy, significantly strengthens the appeal. For example, a patient recovering from a stroke might submit documentation demonstrating ongoing difficulties with balance and coordination, impacting their ability to perform daily activities safely and independently. A supporting letter from the physician could detail how continued physical therapy directly addresses these deficits, reducing fall risk and improving overall functional independence, thereby justifying the need for extended care. A disorganized or poorly substantiated appeal is less likely to succeed, highlighting the importance of meticulous preparation and a clear understanding of the appeals criteria outlined in the insurance policy.
A well-defined appeals process provides essential recourse for individuals seeking medically necessary physical therapy services beyond initial authorizations. Understanding the process, including required documentation, deadlines, and potential levels of appeal, is crucial for effectively advocating for continued care and optimizing recovery outcomes. While appeals processes can be complex and time-consuming, successful navigation often hinges on meticulous preparation, persuasive communication, and a clear demonstration of the link between extended therapy and tangible functional improvements. Failure to effectively utilize this process can result in denied claims and compromised rehabilitation potential, underscoring the importance of proactive engagement and a comprehensive understanding of individual policy provisions. Ultimately, the appeals process plays a crucial role in ensuring access to appropriate levels of care, contributing significantly to the broader objective of maximizing functional recovery and improving quality of life.
6. Alternative Therapies
Exploring alternative therapies within the context of maximizing insurance benefits for physical rehabilitation requires a nuanced understanding of policy limitations and cost-effectiveness. When standard, one-on-one physical therapy sessions reach pre-authorized limits or are deemed medically unnecessary beyond a certain point by the insurer, alternative therapies can serve as a strategic bridge to maintain progress toward functional goals while navigating coverage constraints. This approach necessitates a collaborative discussion between the patient, the prescribing physician, and the physical therapist to identify suitable alternatives aligned with individual needs and policy allowances. For instance, if insurance coverage for individual sessions is exhausted, transitioning to a supervised group exercise program or incorporating a home exercise program, supplemented by periodic check-ins with the therapist, could offer a cost-effective solution to maintain momentum toward recovery while respecting policy limitations. The strategic integration of alternative therapies demonstrates proactive engagement in the rehabilitation process and a commitment to maximizing available resources.
Alternative therapies encompass a range of modalities, each offering distinct advantages and limitations. Home exercise programs, often guided by therapist-prescribed protocols, empower individuals to actively participate in their recovery outside the clinical setting, promoting self-management and potentially reducing the need for costly one-on-one sessions. Group therapy sessions offer a supportive environment for skill development and peer interaction while often incurring lower costs than individual treatment. Telehealth platforms provide remote access to therapeutic guidance, potentially overcoming geographical barriers and scheduling constraints. However, alternative therapies must be carefully considered in light of individual needs and clinical appropriateness. A patient recovering from a complex surgical procedure requiring intensive hands-on therapy might not benefit as significantly from a home exercise program as someone with a less severe injury. Therefore, the selection of alternative therapies must be guided by a thorough assessment of the patient’s condition, functional limitations, and overall treatment goals. For example, a patient with chronic low back pain might benefit from a combination of home exercises, group therapy sessions focused on core strengthening, and periodic telehealth consultations for pain management strategies, offering a comprehensive and cost-effective approach to long-term symptom management. This integrated approach maximizes benefit while potentially reducing reliance on costly individual sessions.
Successfully integrating alternative therapies into a physical rehabilitation plan requires careful consideration of several key factors. Clear communication between the patient, the physician, and the therapist is paramount for establishing realistic expectations, identifying suitable alternatives aligned with individual needs and policy limitations, and ensuring continuity of care. Documentation of the rationale for incorporating alternative therapies, their intended benefits, and progress achieved through these modalities further strengthens the case for continued coverage when seeking subsequent authorizations. While alternative therapies offer potential cost savings and flexibility, they do not replace the expertise and individualized attention provided by one-on-one physical therapy in all cases. Recognizing the limitations of alternative therapies and understanding when specialized, individual care is essential is crucial for optimizing recovery outcomes. Therefore, the integration of alternative therapies should be viewed as a strategic component of a comprehensive rehabilitation plan, carefully tailored to individual needs and circumstances, and implemented in close collaboration with healthcare professionals to ensure safe, effective, and cost-efficient progress toward functional goals. Navigating insurance coverage for alternative therapies can present challenges, requiring careful review of policy provisions and open communication with the insurer regarding covered modalities and reimbursement procedures. Addressing these challenges proactively, with clear documentation and justifications for the chosen alternatives, maximizes the likelihood of continued insurance support throughout the rehabilitation process.
Frequently Asked Questions
Obtaining necessary extensions for rehabilitative care often raises important questions. The following addresses common concerns regarding insurance coverage for extended physical therapy services.
Question 1: How does one demonstrate medical necessity for additional physical therapy visits?
Medical necessity is typically demonstrated through comprehensive documentation, including a clear diagnosis, detailed treatment plan, progress notes illustrating functional improvements, and objective measures of progress, such as range of motion assessments, strength testing, and pain scales. This documentation should clearly link continued therapy to the diagnosed condition and demonstrate its direct impact on the individual’s ability to perform daily activities. A physician’s statement supporting the medical necessity of continued care significantly strengthens the request.
Question 2: What role does the prescribing physician play in securing additional visits?
The prescribing physician plays a crucial role in advocating for extended care. Their expertise in assessing the individual’s condition, formulating a treatment plan, and communicating the medical necessity of continued therapy to the insurance provider carries significant weight. Strong physician advocacy, supported by comprehensive documentation, is essential for navigating the pre-authorization or appeals processes successfully.
Question 3: What steps can be taken if the initial request for extended coverage is denied?
If an initial request is denied, individuals have the right to appeal the decision. A successful appeal typically involves submitting a formal appeal letter, accompanied by supporting documentation that strengthens the case for medical necessity. This might include updated progress notes, additional test results, or a more detailed explanation from the physician regarding the functional limitations and the anticipated benefits of continued therapy. Understanding the specific appeals process outlined in the insurance policy is crucial for navigating this stage effectively.
Question 4: Are there alternative therapies to consider if insurance coverage for traditional physical therapy is limited?
Several alternative therapies may be considered if coverage for traditional physical therapy is limited. These could include home exercise programs, group therapy sessions, or telehealth consultations. The suitability of these alternatives depends on the individual’s specific condition, functional limitations, and treatment goals. Discussing these options with the physician and physical therapist is essential to ensure appropriate and effective alternative care.
Question 5: How does pre-authorization work for extended physical therapy services?
Pre-authorization involves obtaining approval from the insurance provider before commencing additional physical therapy sessions beyond the initially authorized limit. This typically requires submitting a request to the insurer, along with supporting documentation that establishes medical necessity. Pre-authorization helps avoid unexpected out-of-pocket expenses and ensures continued coverage for medically necessary care.
Question 6: Where can individuals find specific details regarding their insurance coverage for physical therapy?
Specific details regarding physical therapy coverage can be found in the individual’s insurance policy documents. Reviewing these documents carefully is crucial for understanding coverage limitations, pre-authorization requirements, and appeals processes. Contacting the insurance provider directly can also provide clarification on specific policy details and answer individual questions. Many insurers also offer online portals with detailed policy information.
Proactive engagement with the healthcare system and a clear understanding of insurance policy provisions are essential for successfully securing the necessary physical therapy services for optimal functional recovery. Diligence in these areas often influences favorable outcomes.
Navigating insurance policies and advocating for appropriate care can feel daunting. Several resources can provide additional support and guidance in this process.
Securing Extended Physical Therapy Benefits
Obtaining additional physical therapy sessions under insurance coverage requires a strategic approach encompassing several key elements. Demonstrating medical necessity through comprehensive documentation, including clear diagnostic information, detailed treatment plans, and progress notes illustrating functional improvements, forms the foundation of successful requests. Strong physician advocacy, coupled with a thorough understanding of policy limitations, pre-authorization requirements, and appeals processes, significantly increases the likelihood of securing necessary extensions. Exploring alternative therapies, such as home exercise programs or group sessions, can provide cost-effective solutions when traditional one-on-one therapy reaches coverage limits. Ultimately, proactive engagement with healthcare providers and insurers, coupled with a clear understanding of policy provisions, empowers individuals to effectively advocate for their rehabilitative needs.
Maximizing insurance benefits for physical therapy services directly impacts individuals’ ability to achieve optimal functional recovery. A comprehensive understanding of the strategies outlined herein equips individuals with the knowledge and tools necessary to navigate the complexities of insurance coverage effectively. Proactive planning, meticulous documentation, and persistent advocacy contribute significantly to favorable outcomes, ensuring access to appropriate levels of care and promoting successful rehabilitation journeys. Access to appropriate rehabilitative care remains a critical component of comprehensive healthcare management, and successful navigation of insurance processes significantly influences patient outcomes and overall well-being.