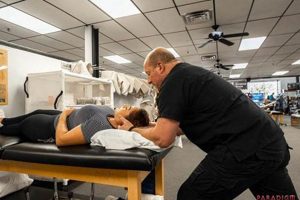
A specialist in kinesiology and exercise science collaborates with patients to improve mobility, manage pain, and restore function after injury or illness. This professional designs individualized fitness programs incorporating therapeutic exercises and activities based on each patient’s specific needs and goals, often working alongside or under the guidance of licensed physical therapists. For example, an individual recovering from knee surgery might work with this type of specialist to rebuild strength and range of motion through targeted exercises.
Restoring physical function and improving overall well-being are paramount concerns in healthcare. Professionals in this field play a vital role in helping individuals regain independence and achieve a higher quality of life. They bridge the gap between rehabilitation and fitness, empowering patients to continue their progress beyond traditional therapy sessions. Historically, the lines between rehabilitation specialists and fitness professionals were more distinct, but the growing recognition of the benefits of exercise in recovery has led to the emergence of this more integrated approach.
The following sections will explore the educational requirements, certifications, and career opportunities associated with this integrated approach to health and fitness, as well as the specific benefits patients can expect to gain from working with these specialists. This includes a closer examination of the collaborative relationship between these professionals and licensed physical therapists, and the various settings in which they practice.
Tips for Maximizing Recovery and Fitness
Individuals seeking improved physical function and overall wellness can benefit from the following practical advice.
Tip 1: Prioritize Proper Posture: Maintaining correct posture throughout daily activities supports musculoskeletal health and reduces the risk of injury. Ergonomic assessments of workspaces and regular postural checks can be beneficial.
Tip 2: Incorporate Regular Stretching: Flexibility is crucial for optimal movement and injury prevention. Dynamic stretching before activity and static stretching afterward improves range of motion and reduces muscle soreness.
Tip 3: Focus on Gradual Progression: Exercise intensity and duration should be increased incrementally to avoid strain and promote sustainable progress. Overexertion can hinder recovery and increase the risk of setbacks.
Tip 4: Maintain Consistent Hydration: Proper hydration is essential for optimal muscle function, joint lubrication, and overall recovery. Adequate water intake supports physiological processes crucial for tissue repair and growth.
Tip 5: Ensure Adequate Rest and Recovery: Rest is as important as exercise for tissue repair and growth. Overtraining can lead to plateaus and increase the risk of injury. Adequate sleep and rest days are crucial for optimal recovery.
Tip 6: Prioritize Proper Nutrition: A balanced diet rich in protein, complex carbohydrates, and healthy fats provides the necessary nutrients for tissue repair, muscle growth, and overall well-being. Nutritional deficiencies can impede recovery and hinder progress.
Tip 7: Listen to Your Body: Recognizing and respecting pain signals is crucial for avoiding further injury. Pushing through pain can exacerbate existing issues and hinder recovery. Modifying activity or seeking professional guidance when experiencing pain is essential.
By adhering to these guidelines, individuals can optimize their physical function, minimize risk of injury, and improve overall well-being. Consistent application of these principles contributes significantly to long-term health and fitness.
In conclusion, the combination of professional guidance and proactive self-care empowers individuals to achieve lasting improvements in physical health and overall quality of life. The subsequent section will explore the importance of ongoing assessment and adaptation in maintaining progress toward individual fitness goals.
1. Rehabilitation
Rehabilitation forms a cornerstone of the services provided by specialists working at the intersection of physical therapy and personal training. It represents the process of restoring lost physical function, mitigating pain, and improving overall quality of life following injury, illness, or surgery. Understanding the multifaceted nature of rehabilitation is crucial for appreciating the expertise these professionals bring to patient care.
- Restoring Functional Movement
Restoring functional movement is a primary objective. This involves addressing impairments in mobility, strength, balance, and coordination through targeted therapeutic exercises and activities. For example, a patient recovering from a stroke might engage in exercises to regain upper limb function and improve balance. This focus on functional restoration allows individuals to regain independence in daily activities.
- Pain Management
Pain management is an integral component. Chronic pain can significantly impact an individual’s quality of life, limiting activity and participation. These professionals implement strategies to alleviate pain through modalities like therapeutic exercise, manual therapy techniques, and education on pain management strategies. This comprehensive approach aims to reduce pain levels and improve overall comfort.
- Injury Prevention
Injury prevention plays a crucial role. By addressing underlying biomechanical imbalances and improving movement patterns, these professionals help patients minimize their risk of future injuries. This proactive approach often involves educating patients on proper body mechanics, ergonomic principles, and appropriate exercise techniques. By empowering patients with knowledge and skills, they foster long-term musculoskeletal health.
- Adaptation and Progression
Adaptation and progression are key principles guiding rehabilitation programs. As patients progress, exercises and activities are adapted to meet their evolving needs and capabilities. This individualized approach ensures that the rehabilitation program remains challenging yet safe, fostering continued improvement and preventing plateaus. Regular assessments allow for adjustments based on individual progress and goals.
These interconnected facets of rehabilitation highlight the comprehensive approach taken by professionals working at the nexus of physical therapy and personal training. By integrating principles of exercise science and rehabilitation, they empower individuals to regain function, manage pain, and achieve optimal physical well-being. This integrated approach ultimately contributes to improved long-term health outcomes and an enhanced quality of life for patients.
2. Exercise Prescription
Exercise prescription represents a cornerstone of the services provided by professionals operating at the intersection of physical therapy and personal training. It involves the development of individualized exercise programs tailored to a client’s specific needs, goals, and physical limitations. This process considers various factors, including current fitness levels, medical history, and any existing injuries or conditions. A well-designed exercise prescription functions as a roadmap guiding clients toward improved physical function, pain management, and overall well-being. For instance, a client recovering from a rotator cuff injury might receive an exercise prescription emphasizing strengthening and flexibility exercises for the shoulder, promoting healing and restoring function while mitigating the risk of re-injury. Similarly, a client managing chronic low back pain might follow a program focused on core strengthening and postural correction. The exercise prescription serves as a critical link between therapeutic goals and practical application.
The effectiveness of exercise prescription hinges on a thorough assessment of the client’s condition. This involves evaluating range of motion, strength, balance, and functional limitations. Understanding these factors allows for the development of a program that addresses specific needs and promotes safe and effective progress. For example, a client with osteoarthritis might require modifications to traditional exercises to protect affected joints. The exercise prescription must also consider the client’s lifestyle, preferences, and available resources to ensure adherence and maximize the likelihood of success. Regular monitoring and adjustments to the program are crucial for ongoing optimization based on the client’s response and progress. This adaptive approach ensures the continued effectiveness of the prescribed exercises.
Integrating exercise prescription within the broader context of physical rehabilitation underscores the importance of a holistic approach to patient care. Challenges may include client adherence to the program and effective communication between the professional and the client. Addressing these challenges requires clear instructions, ongoing support, and regular communication to ensure the client understands the rationale behind the prescribed exercises and feels empowered to actively participate in their recovery journey. Ultimately, the goal of exercise prescription is to facilitate long-term health and wellness by equipping clients with the knowledge and skills to maintain their physical well-being beyond the formal rehabilitation setting.
3. Individualized Programs
Individualized programs represent a cornerstone of effective interventions provided by specialists working at the nexus of physical therapy and personal training. Unlike generic fitness routines, these programs are meticulously tailored to address the unique needs, goals, and physical limitations of each individual. This personalized approach is essential for optimizing outcomes and ensuring both safety and efficacy throughout the rehabilitation or training process. The following facets highlight the key components and implications of individualized programs within this specialized field.
- Needs Assessment
A comprehensive needs assessment forms the foundation of any individualized program. This involves a thorough evaluation of the individual’s current physical condition, medical history, movement patterns, postural alignment, and any existing injuries or limitations. This assessment may include range of motion testing, strength assessments, and functional movement screens. For example, an individual recovering from a shoulder injury would undergo a specific assessment of shoulder mobility and strength to identify deficits and inform exercise selection. The needs assessment provides the crucial data upon which the entire program is built.
- Goal Setting
Establishing clear and attainable goals is essential for maintaining motivation and measuring progress. Goals should be specific, measurable, achievable, relevant, and time-bound (SMART). For example, a client might aim to increase their squat weight by a specific percentage within a defined timeframe, or improve their running distance without pain. Collaboratively setting goals empowers individuals and fosters a sense of ownership over their rehabilitation or training journey. These goals also guide the selection of appropriate exercises and activities.
- Exercise Selection and Progression
Based on the needs assessment and established goals, exercises are carefully selected to address specific impairments and promote functional improvements. The chosen exercises might include strength training, flexibility exercises, balance training, and cardiovascular conditioning, tailored to the individual’s capabilities and limitations. Progression is implemented systematically, gradually increasing the intensity, duration, or complexity of exercises as the individual adapts and improves. This progressive overload principle stimulates ongoing adaptation and prevents plateaus in progress.
- Monitoring and Adaptation
Ongoing monitoring and adaptation are critical for ensuring program effectiveness and safety. Regular assessments track progress towards goals and identify any emerging challenges. The program is adjusted as needed based on the individual’s response to exercise, pain levels, and any changes in their physical condition. For example, if an individual experiences pain during a specific exercise, modifications are made or alternative exercises are prescribed to ensure safe and effective training. This dynamic approach maximizes outcomes and minimizes the risk of setbacks.
These interconnected facets of individualized programs underscore the importance of a personalized approach in promoting optimal physical function and well-being. By tailoring interventions to meet the unique needs of each individual, specialists in this field empower clients to achieve meaningful progress towards their goals, enhance their quality of life, and maintain long-term physical health. This approach distinguishes these professionals from those offering generic fitness solutions and underscores their commitment to evidence-based practice and client-centered care.
4. Improved Functionality
Improved functionality represents a central objective within the scope of a physical therapy personal trainer. It encompasses the restoration and enhancement of physical capacity across a range of activities, from basic daily tasks to complex movements required for specific sports or occupations. Addressing functional limitations is crucial for improving quality of life and enabling individuals to participate fully in desired activities. Understanding the multifaceted nature of improved functionality provides insights into the comprehensive approach taken by these professionals.
- Activities of Daily Living (ADLs)
Restoring and improving the ability to perform activities of daily living (ADLs), such as dressing, bathing, and eating, is a fundamental aspect of improved functionality. A physical therapy personal trainer designs exercise programs that address specific limitations impacting ADLs. For example, an individual recovering from a hip replacement may work on exercises to improve hip mobility and strength, enabling them to perform tasks like putting on shoes or getting in and out of a car with greater ease and independence. Improved ADL performance significantly enhances an individual’s autonomy and overall quality of life.
- Occupational Demands
Addressing functional limitations related to occupational demands is crucial for individuals seeking to return to work or improve their work performance. A physical therapy personal trainer considers the specific physical requirements of a client’s job and develops exercises to improve strength, endurance, and movement patterns relevant to their occupation. For example, a construction worker might focus on exercises to strengthen their back and improve lifting mechanics, while an office worker might work on exercises to improve posture and alleviate repetitive strain injuries. Meeting occupational demands without pain or limitation promotes job satisfaction and long-term career sustainability.
- Recreational Activities
Enabling individuals to participate in recreational activities they enjoy is a key component of improved functionality. Whether it’s playing a sport, gardening, or simply taking a walk, these activities contribute significantly to overall well-being and quality of life. A physical therapy personal trainer develops programs to address limitations hindering participation in these activities. For example, a runner recovering from a knee injury might engage in exercises to improve knee stability and running mechanics, while a golfer might focus on exercises to improve rotational power and flexibility. Restoring recreational capacity enhances physical and mental well-being.
- Movement Quality and Efficiency
Improving overall movement quality and efficiency is central to enhancing functionality. This involves optimizing movement patterns, reducing compensatory movements, and promoting proper biomechanics. By addressing underlying movement dysfunctions, a physical therapy personal trainer helps individuals move with greater ease, efficiency, and reduced risk of injury. For example, an individual with poor posture might undergo exercises to strengthen core muscles and improve spinal alignment, leading to better balance and reduced strain on the neck and back. Improved movement quality translates to better performance and reduced risk of injury in various activities.
These interconnected facets of improved functionality illustrate the comprehensive and individualized approach taken by a physical therapy personal trainer. By addressing limitations across a spectrum of activities and focusing on both physical capacity and movement quality, these professionals empower individuals to regain independence, pursue their goals, and achieve a higher quality of life. This focus on functionality differentiates this approach from generic fitness programs and highlights its relevance in promoting lasting health and well-being.
5. Pain Management
Pain management constitutes a critical component within the scope of a physical therapy personal trainer. Addressing pain, whether acute or chronic, is essential for restoring function, improving quality of life, and facilitating engagement in therapeutic exercise. This involves a multi-faceted approach encompassing identification of pain sources, implementation of appropriate interventions, and education on self-management strategies. The relationship between pain management and the expertise of a physical therapy personal trainer is integral to achieving positive client outcomes. For instance, a client presenting with chronic low back pain might undergo a thorough assessment to identify contributing factors such as muscle imbalances, postural deviations, or movement dysfunctions. The trainer then develops a targeted exercise program addressing these issues, incorporating modalities like stretching, strengthening, and core stabilization exercises. Concurrent education on proper body mechanics and pain management techniques empowers the client to actively participate in their recovery.
Effective pain management often requires a collaborative approach, involving communication with other healthcare professionals, such as physicians, physical therapists, and pain specialists. This interdisciplinary approach ensures comprehensive care and addresses all aspects of the client’s condition. For example, a client experiencing pain related to a recent injury might require referral to a physician for further evaluation or imaging. The physical therapy personal trainer collaborates with the physician to develop a safe and effective exercise program consistent with the client’s medical needs. Similarly, collaboration with a registered dietitian might be beneficial for clients experiencing pain exacerbated by inflammation, ensuring dietary strategies support the overall pain management plan. This collaborative approach optimizes outcomes and provides a comprehensive framework for addressing complex pain conditions.
Integrating pain management principles into exercise prescription and program design is crucial for achieving sustainable results. Understanding the interplay between pain, movement, and function enables the trainer to design programs that promote healing, reduce pain, and improve overall physical capacity. Challenges in pain management can include accurately identifying pain sources, managing client expectations, and addressing psychological factors influencing pain perception. Successfully navigating these challenges necessitates ongoing assessment, open communication, and a client-centered approach emphasizing education and empowerment. Ultimately, effective pain management contributes significantly to improved client outcomes, fostering long-term health, well-being, and enhanced quality of life.
6. Injury Prevention
Injury prevention represents a crucial aspect of the services provided by professionals operating at the intersection of physical therapy and personal training. Proactive strategies to mitigate injury risk are essential for maintaining long-term health, optimizing physical performance, and preventing setbacks in rehabilitation or training programs. Understanding the principles of injury prevention and their practical application is fundamental to the expertise offered by these professionals. This involves a comprehensive approach encompassing movement analysis, exercise modification, and client education.
- Movement Analysis and Correction
Thorough movement analysis identifies biomechanical deficiencies and movement patterns that increase injury susceptibility. Evaluating posture, gait, and functional movement patterns provides insights into potential risk factors. For example, observing excessive pronation during walking or running might indicate an increased risk of ankle, knee, or hip injuries. Corrective exercises and strategies, such as strengthening specific muscle groups or improving flexibility, address these deficiencies and promote safer movement patterns. This proactive approach minimizes the likelihood of injuries stemming from biomechanical imbalances.
- Exercise Modification and Progression
Modifying exercises to accommodate individual limitations and progressing gradually minimizes stress on vulnerable tissues and reduces injury risk. For instance, an individual with a history of low back pain might benefit from modified squatting techniques that minimize spinal loading. Progression of exercises should be gradual and based on individual adaptation, avoiding sudden increases in intensity or volume that could overstress tissues. Appropriate warm-up and cool-down routines further mitigate injury risk by preparing the body for activity and facilitating recovery.
- Client Education and Empowerment
Educating clients about proper body mechanics, safe exercise techniques, and the importance of listening to their bodies empowers them to actively participate in injury prevention. Understanding proper lifting techniques, maintaining correct posture during daily activities, and recognizing early warning signs of injury are essential for long-term musculoskeletal health. Empowered clients are better equipped to make informed decisions about their physical activity and avoid potentially harmful movements or activities. This proactive approach extends injury prevention strategies beyond the training environment and integrates them into daily life.
- Warm-up and Cool-down Protocols
Implementing appropriate warm-up and cool-down protocols prepares the body for activity and facilitates recovery, reducing the risk of injury. A dynamic warm-up, incorporating movements specific to the planned activity, increases blood flow to muscles, improves joint mobility, and prepares the neuromuscular system for exertion. Following activity with a cool-down, including static stretching, helps to reduce muscle soreness, improve flexibility, and promote recovery. These protocols are integral components of comprehensive injury prevention strategies.
These interconnected facets of injury prevention highlight the proactive and comprehensive approach taken by professionals working at the intersection of physical therapy and personal training. By combining movement analysis, exercise modification, client education, and appropriate warm-up and cool-down protocols, they empower individuals to minimize injury risk, optimize physical function, and achieve long-term health and well-being. This emphasis on injury prevention distinguishes their approach from generic fitness programs and underscores the importance of a holistic, individualized approach to exercise and rehabilitation.
Frequently Asked Questions
This section addresses common inquiries regarding the role and services of a specialist integrating physical therapy principles with personalized fitness training.
Question 1: What distinguishes a specialist in this field from a traditional personal trainer or physical therapist?
These specialists bridge the gap between rehabilitation and fitness. They possess expertise in therapeutic exercise and individualized program design, enabling them to address specific functional limitations and facilitate recovery from injury or illness. Unlike traditional personal trainers, they possess a deeper understanding of therapeutic exercise principles. Unlike physical therapists, their focus often extends beyond the initial rehabilitation phase to encompass long-term fitness and wellness.
Question 2: What qualifications should one look for when seeking this type of professional?
Relevant qualifications might include certifications in exercise science, kinesiology, or related fields, along with specialized training in therapeutic exercise. Experience working with individuals recovering from injuries or managing chronic conditions is also valuable. Verification of credentials and licensure, where applicable, should always be performed.
Question 3: Is a physician referral required to engage the services of this type of specialist?
While a physician referral is not always mandatory, it is often recommended, especially for individuals with pre-existing medical conditions or recent injuries. Collaboration with healthcare providers ensures a coordinated approach to care and maximizes client safety.
Question 4: What types of conditions can this type of specialist address?
These professionals can work with individuals experiencing a range of conditions, including musculoskeletal injuries, post-surgical rehabilitation, chronic pain, and neurological conditions. Their expertise extends to improving functional capacity, managing pain, and enhancing overall physical well-being.
Question 5: What should one expect during an initial consultation with this type of specialist?
An initial consultation typically involves a comprehensive assessment of the individual’s current physical condition, medical history, and goals. This may include movement assessments, postural evaluations, and discussions regarding lifestyle and limitations. The consultation provides a foundation for developing an individualized program.
Question 6: How does the cost of these services compare to traditional personal training or physical therapy?
Cost varies depending on factors such as location, experience, and specific services provided. Generally, these services are positioned between personal training and physical therapy in terms of cost, reflecting the specialized expertise and individualized nature of care.
Engaging a qualified professional can significantly benefit individuals seeking to improve physical function, manage pain, and achieve their fitness goals. Thorough research and consideration of individual needs are crucial when selecting a provider.
The following section explores case studies demonstrating the practical application and positive outcomes achieved through individualized programs designed by these specialized professionals.
Conclusion
This exploration of the evolving role of specialists integrating physical therapy and personal training has highlighted the significant benefits conferred upon individuals seeking improved physical function, pain management, and enhanced well-being. Key takeaways include the importance of individualized programs tailored to specific needs and limitations, the emphasis on corrective exercise and movement re-education, and the collaborative approach often employed to ensure comprehensive client care. The integration of therapeutic exercise principles with personalized fitness programming offers a valuable pathway toward achieving optimal physical health and functional capacity. From post-rehabilitation recovery to proactive injury prevention, this specialized approach addresses a spectrum of needs within the healthcare and fitness continuum.
As the demand for integrated health and wellness solutions continues to grow, the role of professionals bridging the gap between physical therapy and personal training assumes increasing significance. This specialized expertise offers a valuable resource for individuals seeking to optimize physical function, manage pain, and improve overall quality of life. Further research and development within this field promise continued advancements in personalized exercise interventions and injury prevention strategies, ultimately contributing to enhanced health outcomes and empowering individuals to achieve their full physical potential.