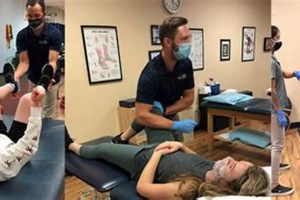
Specialized seating designed for rehabilitation and treatment offers support, adjustability, and specific features to facilitate therapeutic exercises, improve posture, and enhance patient comfort during recovery. For instance, a chair with adjustable height and backrests can be tailored to an individual’s needs for optimal positioning during specific exercises.
Such adaptable furniture plays a vital role in various healthcare settings, enabling safer and more effective treatment for patients with mobility limitations or recovering from injuries. Historically, therapeutic seating evolved from basic designs to incorporate ergonomic principles and advanced mechanisms, reflecting a growing understanding of patient needs and therapeutic effectiveness. This evolution has led to improvements in patient outcomes and overall quality of care.
Further exploration of this topic will cover specific design features, diverse applications in different therapeutic contexts, and the selection criteria for choosing appropriate seating to meet individual patient requirements.
Tips for Utilizing Specialized Therapeutic Seating
Proper use of adapted seating optimizes therapeutic benefits and promotes patient safety and comfort. Consider these guidelines for effective utilization:
Tip 1: Adjustability is Key: Ensure the chair’s height, backrest angle, and other adjustable components are tailored to the individual’s specific needs and the requirements of the therapy being administered. Proper adjustment facilitates correct posture and movement.
Tip 2: Stability and Safety: Verify chair stability before use. Confirm locking mechanisms are engaged and weight capacity is appropriate for the individual. These precautions prevent accidents and ensure a safe therapeutic environment.
Tip 3: Consider Specific Needs: Select seating with features that address individual requirements, such as pressure relief cushions for those at risk of pressure sores, or specialized armrests and footrests for enhanced support and stability.
Tip 4: Proper Positioning and Posture: Encourage correct posture while seated. Ensure proper alignment of the spine, hips, and knees to maximize comfort and minimize strain during therapy sessions.
Tip 5: Regular Maintenance: Inspect the chair regularly for wear and tear. Address any necessary repairs promptly to maintain safety and functionality. Lubricate moving parts as needed.
Tip 6: Cleanliness and Hygiene: Establish and maintain a cleaning protocol for the chair to prevent the spread of infection. Use appropriate disinfectants and follow manufacturer guidelines for cleaning and maintenance.
Tip 7: Training and Education: Healthcare professionals should receive adequate training on the proper use and adjustment of therapeutic seating. This ensures safe and effective application of the equipment.
Following these guidelines ensures safe, comfortable, and effective use of specialized seating, contributing significantly to positive therapeutic outcomes.
By understanding the importance of proper utilization and selection, healthcare providers can effectively integrate specialized seating into treatment plans, leading to improved patient well-being and functional independence.
1. Adjustability
Adjustability is a crucial feature in therapeutic seating, directly impacting the effectiveness of treatment and patient comfort. Adaptable components allow customization to individual needs and therapeutic goals, facilitating proper posture, exercise execution, and overall well-being.
- Height Adjustment
Variable height accommodates diverse patient statures and facilitates transfers. A chair easily adjusted to match a patient’s leg length promotes safe and comfortable transitions. This feature is essential for individuals with limited mobility and those recovering from lower extremity injuries.
- Backrest Angle
Adjustable backrests support a variety of postures required for different therapeutic exercises and interventions. The ability to recline or incline the backrest promotes proper spinal alignment, reduces pressure, and optimizes comfort during treatment sessions. This feature is particularly important for patients with back pain or postural issues. For example, a more upright position might be beneficial for strengthening exercises, while a reclined position may be needed for relaxation or pain relief.
- Leg Rest and Footrest Adjustments
Adaptable leg rests and footrests accommodate varying leg lengths and promote proper lower extremity positioning. This is crucial for maintaining circulation, reducing swelling, and supporting comfortable positioning during exercises. Independent adjustments for each leg can be vital for patients with asymmetrical conditions or unilateral injuries.
- Armrest Adjustments
Adjustable armrests provide support and stability during transfers and therapeutic activities. They can be adjusted in height, width, and angle to accommodate individual needs and preferences. This feature is particularly helpful for patients with upper extremity weakness or limited range of motion, providing stability and assistance during exercises.
These adjustable features contribute significantly to the therapeutic value of specialized seating. Proper customization allows therapists to create optimal positioning for individual patients, supporting effective treatment interventions and maximizing comfort throughout the rehabilitation process. The ability to tailor the chair to specific requirements enhances patient engagement and facilitates improved therapeutic outcomes.
2. Support
Supportive seating is fundamental to effective physical therapy. Proper support enhances patient comfort, facilitates correct posture, and enables safe and effective therapeutic interventions. It forms the foundation for successful rehabilitation by stabilizing the body, reducing strain, and promoting optimal biomechanics.
- Postural Alignment
Specialized chairs provide essential support to maintain correct postural alignment during therapy. Proper back and lumbar support reduces strain on the spine, promoting comfort and preventing further injury. This is crucial for patients recovering from back injuries, surgeries, or those with chronic postural issues. For example, contoured backrests and adjustable lumbar supports can accommodate individual spinal curvatures, ensuring proper weight distribution and reducing pressure points.
- Weight Distribution
Effective support distributes weight evenly, minimizing pressure on vulnerable areas and reducing the risk of pressure sores. This is particularly important for patients with limited mobility or those who spend extended periods seated. Specialized cushions and pressure-relieving materials contribute to enhanced comfort and skin integrity. A well-designed seat cushion, for example, can distribute weight across the buttocks and thighs, reducing pressure on the coccyx and ischial tuberosities.
- Enhanced Stability
Supportive seating provides stability, enabling patients to engage in therapeutic exercises with confidence and control. Secure and stable positioning reduces the risk of falls and allows for focused movement during rehabilitation. This is especially important for patients with balance impairments or weakened muscles. Features such as sturdy frames, wide bases, and secure armrests contribute to overall stability and safety.
- Reduced Pain and Discomfort
Proper support alleviates pain and discomfort, allowing patients to participate more fully in therapy sessions. By minimizing strain on joints and muscles, supportive seating promotes relaxation and enhances the effectiveness of therapeutic interventions. For patients with chronic pain conditions, adequate support can be essential for tolerating and benefiting from therapy. Adjustable features and customizable support options cater to individual needs and sensitivities.
These facets of support contribute significantly to the overall effectiveness of physical therapy. By providing a stable, comfortable, and supportive foundation, specialized seating enables patients to engage more actively in their rehabilitation, facilitating progress toward functional independence and improved well-being.
3. Safety
Safety is paramount in therapeutic settings. A properly designed and utilized physical therapy chair minimizes risks and contributes to a secure environment conducive to effective rehabilitation. Careful consideration of safety features and proper usage protocols are essential for both patients and healthcare professionals.
- Stability
Chair stability is crucial for preventing falls and injuries. A stable base, robust construction, and secure locking mechanisms prevent tipping or shifting during use. For example, a chair with a wider base and non-slip feet provides greater stability than one with a narrow base or smooth feet. This is particularly important for patients with balance issues or weakened muscles.
- Weight Capacity
Adhering to the chair’s specified weight capacity is essential. Exceeding this limit compromises structural integrity and increases the risk of collapse. Assessing patient weight and selecting appropriate seating ensures safety and prevents equipment failure. For instance, bariatric chairs are designed to accommodate heavier individuals safely.
- Locking Mechanisms
Functional locking mechanisms secure adjustable components, preventing unintended movement during therapy. Ensuring these mechanisms are engaged before and during use maintains stability and prevents accidental adjustments that could compromise patient safety. Regular inspection and maintenance of these mechanisms are crucial for reliable function.
- Emergency Preparedness
Incorporating safety features like quick-release mechanisms on adjustable components facilitates rapid response in emergencies. These features enable caregivers to quickly adjust the chair or evacuate patients in critical situations, such as medical emergencies or fire evacuations.
These safety considerations are integral to the design and utilization of effective therapeutic seating. Prioritizing these aspects creates a secure environment that promotes patient well-being and facilitates successful rehabilitation outcomes. Neglecting these elements can lead to accidents, injuries, and compromised therapeutic effectiveness.
4. Comfort
Comfort in therapeutic seating plays a crucial role in patient compliance, treatment efficacy, and overall well-being. Discomfort can hinder patient engagement, limit participation in prescribed exercises, and negatively impact therapeutic outcomes. Conversely, a comfortable chair promotes relaxation, reduces anxiety, and encourages active participation in the rehabilitation process. For example, a patient experiencing back pain is more likely to engage fully in therapeutic exercises if seated comfortably, allowing for focused effort and improved adherence to treatment plans. Furthermore, enhanced comfort during prolonged therapy sessions contributes to a positive patient experience, fostering motivation and a sense of progress. The relationship between comfort and effective rehabilitation is symbiotic; improved comfort enhances therapeutic efficacy, while successful therapy, in turn, contributes to greater overall well-being and comfort.
Several factors contribute to seating comfort, including proper cushioning, ergonomic design, and adjustability. Adequate cushioning distributes pressure evenly, reducing stress on vulnerable areas and preventing pressure sores. Ergonomic design supports natural body posture, minimizing strain on joints and muscles. Adjustability allows customization to individual body types and specific therapeutic needs, accommodating varying heights, weights, and postural requirements. For instance, a chair with adjustable lumbar support can be tailored to accommodate the individual’s spinal curvature, reducing back pain and promoting proper posture during therapy. These features work in concert to create a supportive and comfortable seating experience that enhances therapeutic effectiveness and promotes patient well-being.
Understanding the impact of comfort on therapeutic outcomes highlights its importance as a key consideration in the design and selection of physical therapy seating. Addressing comfort not only improves patient experience but also contributes directly to successful rehabilitation. While other factors like safety and functionality are critical, neglecting comfort can compromise the overall effectiveness of therapy. Investing in comfortable and supportive seating is an investment in positive patient outcomes and enhanced quality of care. This understanding should inform decisions related to equipment procurement, therapeutic protocols, and overall patient management within rehabilitation settings.
5. Durability
Durability is a critical factor in the efficacy and cost-effectiveness of therapeutic seating. Chairs subjected to frequent use, varied patient weights, and regular adjustments must withstand wear and tear without compromising structural integrity or functional performance. A durable chair minimizes the need for frequent repairs or replacements, reducing long-term costs and ensuring consistent availability for patient care. For example, reinforced frames, robust upholstery, and high-quality mechanisms contribute to a chair’s ability to withstand the demands of a busy therapeutic environment. A lack of durability can lead to premature failure, disruptions in treatment schedules, and increased expenses associated with repairs or replacements. Furthermore, compromised structural integrity poses safety risks to patients and therapists. Selecting durable seating ensures long-term reliability and contributes to a safe and efficient therapeutic setting.
The practical significance of durability extends beyond cost considerations. A durable chair maintains consistent performance, providing reliable support and adjustability throughout its lifespan. This consistency is essential for delivering effective therapy, as it allows therapists to rely on the chair’s functionality and ensures patients receive consistent support during treatment sessions. For instance, a chair with durable upholstery resists tearing and maintains its shape, providing consistent comfort and support over time. Conversely, a chair with low-quality upholstery may quickly become worn and uncomfortable, negatively impacting patient experience and potentially hindering therapeutic progress. Therefore, prioritizing durability ensures the chair remains a reliable tool in the rehabilitation process, contributing to positive patient outcomes and long-term cost savings.
In conclusion, durability in therapeutic seating is an essential factor influencing both practical functionality and economic considerations. Investing in durable chairs ensures long-term reliability, minimizes disruptions in care, and contributes to a safe and effective therapeutic environment. Understanding the relationship between durability and the overall efficacy of physical therapy chairs informs purchasing decisions, optimizes resource allocation, and ultimately supports improved patient care and outcomes. This knowledge empowers healthcare providers to make informed choices that prioritize both patient well-being and responsible resource management.
6. Hygiene
Maintaining hygiene in therapeutic settings is crucial for infection control and patient safety. Physical therapy chairs, frequently used by multiple patients, can become vectors for disease transmission if not properly cleaned and disinfected. Regular cleaning removes visible contaminants like dirt and bodily fluids, while disinfection eliminates harmful microorganisms. This two-step process minimizes the risk of cross-contamination and protects vulnerable patients from healthcare-associated infections. For example, neglecting to clean a chair after a patient with a contagious skin condition could expose subsequent users to infection. Conversely, consistent adherence to hygiene protocols contributes significantly to a safer and healthier therapeutic environment.
Effective hygiene protocols for physical therapy chairs involve several key practices. Selecting appropriate cleaning agents and disinfectants is essential. These products should be effective against a broad spectrum of microorganisms, yet safe for use on the chair’s materials. Following manufacturer guidelines for cleaning and disinfection ensures optimal efficacy without damaging the chair’s surfaces. Proper cleaning techniques, such as wiping down all surfaces thoroughly, including frequently touched areas like armrests and handles, are essential for complete decontamination. Establishing a regular cleaning schedule, based on frequency of use and patient population, ensures consistent hygiene maintenance. For instance, chairs used in high-traffic areas or with patients at higher risk of infection may require more frequent cleaning than those used less frequently or with lower-risk patients. Additionally, prompt cleaning and disinfection after spills or contamination with bodily fluids are crucial for preventing the spread of infection. These practical steps, implemented consistently, contribute to a hygienic and safe environment for both patients and healthcare professionals.
In summary, maintaining hygiene in the context of physical therapy chairs is integral to patient safety and infection control. Consistent application of appropriate cleaning and disinfection protocols minimizes the risk of cross-contamination and promotes a healthy therapeutic environment. Understanding the importance of hygiene in this context and implementing practical measures to uphold these standards are fundamental responsibilities within healthcare settings. Challenges may include resource constraints, staff training, and adherence to protocols, but addressing these challenges proactively through ongoing education and resource allocation ensures a safe and effective therapeutic environment for all. This commitment to hygiene ultimately contributes to improved patient outcomes and a higher standard of care.
7. Specific Needs
Therapeutic seating must address diverse individual requirements to maximize effectiveness. A patient’s specific needs dictate the appropriate chair features, ensuring optimal support, comfort, and therapeutic benefit. Consideration of these needs is crucial for successful rehabilitation outcomes. This section explores various individual requirements and their influence on chair selection.
- Bariatric Considerations
Patients with larger body sizes require specialized seating designed to accommodate their weight and dimensions safely. Bariatric chairs typically feature reinforced frames, wider seats, and higher weight capacities. These adaptations ensure stability, prevent equipment failure, and promote patient comfort and safety during therapy. For instance, a standard chair may not provide adequate support or stability for a bariatric patient, increasing the risk of falls or equipment damage. A bariatric chair, however, addresses these specific needs, ensuring a safe and comfortable therapeutic experience.
- Postural Impairments
Individuals with postural impairments, such as scoliosis or kyphosis, benefit from chairs offering specialized support and alignment features. Adjustable backrests, lumbar supports, and contoured seating surfaces accommodate individual spinal curvatures and promote proper posture. These adaptations reduce strain, enhance comfort, and facilitate effective therapeutic interventions. For example, a patient with scoliosis may require a chair with adjustable lateral supports to accommodate their spinal curvature and promote proper alignment during therapy.
- Pressure Relief
Patients at risk of pressure sores, often due to limited mobility or compromised circulation, require seating designed to minimize pressure points and promote skin integrity. Pressure-relieving cushions, specialized materials, and adjustable seating surfaces distribute weight evenly, reducing pressure on vulnerable areas. This is particularly important for patients with spinal cord injuries, diabetes, or other conditions that compromise circulation and increase the risk of pressure sores. For instance, a patient with a spinal cord injury may benefit from a chair with a pressure-relieving cushion that conforms to their body shape and reduces pressure on bony prominences.
- Limited Mobility and Transfers
Individuals with limited mobility require seating that facilitates safe and easy transfers. Features such as adjustable seat height, swing-away armrests, and removable footrests assist patients in moving to and from the chair. These adaptations minimize strain, reduce the risk of falls, and promote independence during transfers. For example, a patient with limited lower extremity strength may benefit from a chair with a lower seat height and swing-away armrests to facilitate easier transfers.
Addressing specific needs through appropriate chair selection optimizes therapeutic effectiveness and enhances patient well-being. Failing to accommodate these individual requirements can compromise safety, limit participation in therapy, and negatively impact rehabilitation outcomes. Therefore, careful consideration of specific needs is an essential component of providing effective and patient-centered physical therapy services. This attention to individual requirements demonstrates a commitment to personalized care and contributes significantly to positive therapeutic outcomes.
Frequently Asked Questions
This section addresses common inquiries regarding specialized therapeutic seating, providing concise and informative responses to facilitate informed decision-making and optimal utilization.
Question 1: What distinguishes a therapeutic chair from standard seating?
Therapeutic chairs offer specific features designed to support rehabilitation, such as adjustable height, backrests, and leg rests, specialized cushioning for pressure relief, and enhanced stability features. Standard chairs typically lack these adaptations.
Question 2: How does one select the appropriate therapeutic chair for individual needs?
Selection depends on factors such as the patient’s diagnosis, mobility level, weight, postural requirements, and specific therapeutic goals. Consulting with a physical therapist or healthcare professional is recommended to determine the most suitable chair.
Question 3: Are there specific safety considerations when using therapeutic seating?
Adhering to weight capacity limits, engaging locking mechanisms, and ensuring proper chair stability are essential safety precautions. Regular inspections and maintenance are also crucial for safe operation.
Question 4: What are the key benefits of utilizing therapeutic seating in rehabilitation?
Benefits include improved posture, enhanced comfort, reduced pain, increased stability, and facilitated therapeutic exercises. These factors contribute to improved patient outcomes and functional independence.
Question 5: How does proper maintenance contribute to the longevity and effectiveness of therapeutic chairs?
Regular cleaning, lubrication of moving parts, and prompt repair of any damage ensure optimal functionality and extend the lifespan of the chair. Proper maintenance also contributes to hygiene and infection control.
Question 6: Where can reliable information regarding therapeutic seating options be found?
Reputable medical equipment suppliers, healthcare professionals, and specialized rehabilitation resources offer comprehensive information regarding therapeutic seating options and selection criteria.
Understanding these fundamental aspects of therapeutic seating enables informed selection, appropriate utilization, and optimization of therapeutic benefits for patients undergoing rehabilitation.
For further information regarding specific product recommendations or individual needs assessments, consultation with a qualified healthcare professional is advisable.
Conclusion
Specialized seating designed for physical therapy plays a crucial role in rehabilitation. Exploration of this topic encompassed design considerations, emphasizing adjustability, support, safety, comfort, durability, and hygiene. Furthermore, the importance of addressing specific patient needs, such as bariatric requirements, postural impairments, pressure relief, and limited mobility, was highlighted. Effective utilization and proper maintenance ensure optimal therapeutic benefit and contribute to successful rehabilitation outcomes.
Appropriate seating empowers individuals to actively participate in therapy, promoting progress toward functional independence and improved quality of life. Continued advancements in design and technology promise further enhancements in therapeutic seating, leading to more effective rehabilitation interventions and improved patient care.