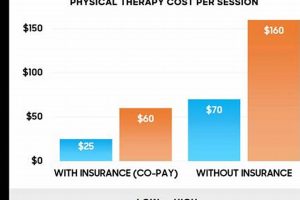
The expense of rehabilitative treatment utilizing insurance coverage varies based on several factors. These include the individual’s specific insurance plan, the type of therapy required, the duration of treatment, the therapist’s location, and whether the provider is in-network or out-of-network. For example, a patient with a Preferred Provider Organization (PPO) plan might pay a copay of $25-$50 per session for an in-network physical therapist, while someone with a high-deductible health plan might be responsible for the full cost of treatment until their deductible is met. Understanding these cost variations is crucial for budgeting and making informed decisions about healthcare.
Accessing affordable rehabilitative care is essential for regaining functional mobility, managing pain, and improving overall quality of life after an injury or illness. Historically, the cost of such care has been a significant barrier for many individuals. The evolution of insurance coverage has made these services more accessible, but navigating the complexities of insurance plans and understanding cost-sharing responsibilities remains a challenge. Informed decision-making regarding coverage and provider networks can significantly impact the financial burden on patients.
This article will delve into the factors influencing the cost of rehabilitative services under insurance coverage. It will explore various insurance plan types and their associated costs, provide strategies for minimizing out-of-pocket expenses, and offer resources for understanding patient rights and responsibilities within the healthcare system.
Tips for Managing Rehabilitation Costs
Managing the expenses associated with rehabilitative care requires careful planning and a thorough understanding of insurance benefits. The following tips provide guidance for navigating this often-complex process.
Tip 1: Review Insurance Policy Details: Carefully examine policy documents to understand coverage specifics for rehabilitative services, including copay amounts, coinsurance percentages, deductible requirements, and out-of-pocket maximums. Contact the insurance provider directly for clarification on any unclear points.
Tip 2: Utilize In-Network Providers: Treatment from in-network providers typically results in lower out-of-pocket expenses. Insurance companies often negotiate discounted rates with preferred providers. Verify provider network participation through the insurer’s website or by contacting customer service.
Tip 3: Explore Pre-Authorization Requirements: Some insurance plans require pre-authorization for certain therapies or a specific number of sessions. Failure to obtain pre-authorization may lead to denial of coverage. Confirm pre-authorization requirements with the insurance provider before commencing treatment.
Tip 4: Consider Treatment Setting Options: The setting where therapy is received (hospital outpatient department, private clinic, home health) can influence costs. Compare pricing across different settings while considering convenience and individual needs.
Tip 5: Inquire About Package Deals or Discounted Rates: Some providers offer package deals for multiple sessions or discounted rates for upfront payments. Explore these options to potentially reduce overall expenses.
Tip 6: Maintain Detailed Records: Keep meticulous records of all appointments, treatments, and billing statements. This documentation can be valuable for tracking expenses, verifying insurance payments, and addressing any billing discrepancies.
Tip 7: Explore Alternative Funding Options: If insurance coverage is limited or unavailable, explore alternative funding options such as health savings accounts (HSAs), flexible spending accounts (FSAs), or payment plans offered by the provider.
By understanding insurance benefits and proactively exploring cost-saving strategies, individuals can effectively manage the financial aspects of rehabilitative care and focus on recovery.
This information provides a foundation for making informed decisions about rehabilitation costs. The concluding section will summarize key takeaways and offer additional resources for navigating the healthcare system.
1. Insurance Plan Type
Insurance plan type significantly influences the out-of-pocket cost of physical therapy. Different plan structures determine how costs are shared between the insurer and the insured. Understanding these variations is crucial for effective financial planning.
Health Maintenance Organizations (HMOs) typically require patients to select a primary care physician (PCP) who acts as a gatekeeper for specialist referrals, including physical therapy. HMOs often feature lower premiums and copays for in-network services, but coverage for out-of-network providers is generally limited or nonexistent. For example, an individual with an HMO might pay a $20 copay for each in-network physical therapy visit, but face the full cost if choosing an out-of-network provider.
Preferred Provider Organizations (PPOs) offer greater flexibility in provider choice. While in-network services are incentivized with lower cost-sharing, PPOs also provide coverage for out-of-network care, albeit at a higher cost. For instance, a PPO plan might require a $30 copay for in-network physical therapy and cover 60% of the cost for out-of-network services, leaving the patient responsible for the remaining 40%. Point-of-Service (POS) plans combine aspects of HMOs and PPOs, requiring a PCP referral but allowing for out-of-network care at a higher cost.
High-deductible health plans (HDHPs) feature lower premiums but require patients to meet a higher deductible before significant coverage begins. This means individuals may be responsible for the full cost of physical therapy until their deductible is met. HDHPs are often paired with health savings accounts (HSAs), which allow pre-tax contributions to be used for qualified medical expenses, including physical therapy.
Finally, understanding the specifics of one’s insurance planincluding coverage limitations, pre-authorization requirements, and maximum benefit allowancesis crucial for managing and predicting the financial implications of physical therapy. This knowledge empowers informed decisions regarding provider selection and treatment planning. Consulting directly with the insurance provider and reviewing policy documents are essential steps in this process.
2. Copays and Coinsurance
Copays and coinsurance are fundamental cost-sharing components within most health insurance plans, directly impacting the out-of-pocket expenses associated with physical therapy. A copay represents a fixed dollar amount paid for each visit, while coinsurance represents a percentage of the cost shared between the patient and insurer after the deductible is met. These mechanisms influence both the predictability and overall expense of treatment.
For instance, a plan with a $25 copay for physical therapy requires the patient to pay this amount for each session, regardless of the total cost. If a session costs $150, the insurer covers the remaining $125. In contrast, a plan with a 20% coinsurance rate, after a $500 deductible, requires the patient to pay 20% of the cost for each session once the deductible is met. If the deductible has been satisfied and a session costs $150, the patient’s responsibility is $30, with the insurer covering $120.
The interplay between copays, coinsurance, and deductibles significantly shapes the total cost burden. Patients with high deductibles and coinsurance may face substantial initial expenses before experiencing the cost-sharing benefits of insurance. Conversely, low copays and minimal coinsurance can make physical therapy more financially accessible, particularly for individuals requiring frequent or long-term treatment. Choosing a plan with appropriate cost-sharing parameters tailored to individual healthcare needs and financial circumstances is crucial for effective cost management.
3. Deductibles
Deductibles represent a crucial component in understanding the overall cost of physical therapy with insurance. A deductible is the amount a patient must pay out-of-pocket before insurance coverage begins to pay for eligible medical expenses. This upfront cost significantly influences the financial burden associated with treatment and requires careful consideration when selecting an insurance plan.
- Annual Deductible
Most insurance plans operate with an annual deductible, which resets at the beginning of each calendar year. Until the deductible is met, the patient bears the full cost of covered services, including physical therapy. For example, if an individual has a $1,000 annual deductible and requires physical therapy costing $150 per session, they will be responsible for the full cost of the first six sessions and a portion of the seventh, until the $1,000 threshold is reached.
- Impact on Treatment Decisions
The deductible amount can significantly influence decisions regarding the timing and extent of physical therapy. A high deductible can deter individuals from seeking timely care, potentially exacerbating existing conditions. Conversely, a lower deductible can encourage early intervention, facilitating faster recovery and potentially reducing long-term healthcare costs. For example, someone with a high deductible may postpone necessary physical therapy due to the initial financial strain, while someone with a lower deductible may be more inclined to initiate treatment promptly.
- Relationship to Premiums
Deductible amounts are typically inversely related to insurance premiums. Plans with higher deductibles often have lower monthly premiums, and vice versa. This trade-off necessitates careful consideration of individual financial circumstances and healthcare needs. Someone anticipating significant healthcare utilization may opt for a lower deductible and higher premium to minimize out-of-pocket expenses throughout the year, while someone anticipating minimal healthcare needs might choose a higher deductible and lower premium.
- Strategies for Managing Deductible Costs
Managing deductible costs requires proactive planning and resource utilization. Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) offer tax-advantaged ways to save for medical expenses, including deductibles. Understanding deductible requirements and incorporating them into budgeting can mitigate the financial impact of necessary healthcare services. Additionally, exploring payment plan options with healthcare providers can alleviate the burden of large upfront costs.
The deductible amount is a critical factor in determining the overall cost of physical therapy with insurance. Carefully evaluating deductible options alongside premium costs and anticipated healthcare needs allows individuals to select insurance plans aligned with their financial capabilities and healthcare goals. Understanding the influence of deductibles on treatment decisions and exploring available resources for managing these costs empowers informed and financially sound healthcare choices.
4. In-network vs. out-of-network
The distinction between in-network and out-of-network physical therapists significantly impacts the cost of treatment under insurance. In-network providers have contracted with insurance companies to provide services at pre-negotiated rates, typically resulting in lower out-of-pocket expenses for patients. Out-of-network providers do not have such agreements, potentially leading to significantly higher costs.
- Cost-Sharing Variations
Cost-sharing for in-network services typically involves lower copays, coinsurance percentages, and deductibles. For example, a patient might pay a $25 copay for an in-network visit, but 50% of the total cost for an out-of-network visit. This difference can substantially affect the overall expense, especially for multiple sessions. Insurance companies often provide online directories or customer service lines to verify provider network status.
- Reimbursement Rates and Balance Billing
Insurance companies reimburse out-of-network providers at a lower rate than in-network providers. The difference between the provider’s charge and the insurance reimbursement can be “balance billed” to the patient, resulting in unexpected and potentially high expenses. For instance, if a therapist charges $200 and the insurance company reimburses $80, the patient may be responsible for the remaining $120. This practice is less common with in-network providers due to pre-negotiated rates. Understanding balance billing practices is crucial for managing out-of-network costs.
- Impact on Provider Choice
Network restrictions limit patient choice to providers within the insurance plan’s network. While offering cost savings, this may prevent access to preferred therapists or specialists outside the network. Balancing cost considerations with desired provider access is essential when selecting an insurance plan and navigating treatment options. This choice may involve weighing the financial benefits of in-network care against the potential advantages of a specific out-of-network provider’s expertise.
- Exceptions and Pre-Authorization
Some insurance plans allow exceptions for out-of-network care under specific circumstances, such as a lack of in-network specialists for a particular condition. Pre-authorization from the insurance company is often required in these cases. Securing pre-authorization involves demonstrating medical necessity and may require additional documentation. Navigating this process effectively is essential to ensure coverage and avoid unexpected costs for out-of-network services deemed medically necessary.
The choice between in-network and out-of-network physical therapy directly affects the cost of treatment. Understanding the nuances of cost-sharing, reimbursement rates, provider choice limitations, and pre-authorization requirements empowers informed decisions aligned with individual healthcare needs and financial circumstances. Considering these factors within the broader context of insurance plan selection and treatment planning ensures cost-effective access to quality care.
Pre-authorization requirements play a significant role in determining the out-of-pocket cost of physical therapy for insured individuals. This process, where the insurer approves treatment before it begins, impacts both access to care and the potential for unexpected expenses. Understanding pre-authorization policies is crucial for effective cost management and informed treatment planning.
- Necessity of Pre-authorization
Insurance companies often require pre-authorization for certain types of physical therapy, particularly those involving extensive treatment plans, specialized techniques, or non-routine interventions. This requirement stems from the insurer’s need to assess the medical necessity and cost-effectiveness of the proposed treatment. Failure to obtain pre-authorization can lead to denial of coverage, leaving the patient responsible for the full cost of services. For instance, a patient needing specialized manual therapy for a complex condition might require pre-authorization, while a patient with a routine ankle sprain might not. This distinction highlights the importance of verifying pre-authorization requirements before commencing treatment.
- Process and Timeline
The pre-authorization process typically involves the physical therapist submitting detailed documentation to the insurance company, outlining the patient’s diagnosis, treatment plan, and anticipated duration of care. The insurer then reviews this information to determine if the proposed treatment aligns with their coverage policies. This process can take several days or even weeks, potentially delaying the start of therapy. Understanding these timelines is crucial for managing patient expectations and coordinating care effectively. Delays in pre-authorization can impact treatment initiation and necessitate open communication between the patient, therapist, and insurer.
- Potential for Denial and Appeals
Pre-authorization requests can be denied if the insurer deems the proposed treatment medically unnecessary, experimental, or exceeding established coverage limits. Denials can be appealed, but the appeals process can be time-consuming and complex, requiring further documentation and justification. Patients facing denials should understand their appeal rights and seek assistance from their therapist or insurance provider to navigate this process. Successful appeals can reinstate coverage, while unsuccessful appeals may leave the patient responsible for the full cost, emphasizing the importance of thorough documentation and clear communication with the insurer.
- Impact on Treatment Planning and Cost
Pre-authorization requirements influence treatment planning by establishing coverage parameters and potentially limiting the number of approved sessions or the types of interventions covered. This can impact the overall cost of care by either restricting access to potentially beneficial services or shifting the financial burden onto the patient. For example, if pre-authorization is granted for only a limited number of sessions, the patient might incur additional out-of-pocket expenses for further necessary treatment. Understanding these limitations allows patients to explore alternative treatment options or financial assistance programs if necessary.
Pre-authorization requirements are integral to understanding the cost of physical therapy with insurance. Navigating these requirements effectively, including verifying necessity, understanding the process, and managing potential denials, is crucial for both accessing necessary care and controlling out-of-pocket expenses. Pre-authorization serves as a gatekeeping mechanism, impacting both the financial and logistical aspects of physical therapy treatment. Integrating pre-authorization considerations into treatment planning and insurance selection empowers informed decision-making and facilitates a smoother healthcare experience.
6. Number of Sessions Needed
The required number of physical therapy sessions directly influences the overall cost of treatment under insurance. Treatment duration hinges on the complexity of the condition, individual response to therapy, and the desired functional outcome. A longer treatment duration, necessitating more sessions, inherently increases the cumulative cost, impacting both insurer payments and patient out-of-pocket expenses. This correlation necessitates careful consideration of treatment plans and cost projections. For example, a patient recovering from a simple strain might require only a few sessions, incurring minimal cost, whereas a patient rehabilitating from a complex surgical procedure might require months of therapy, leading to significantly higher expenses.
Insurance plans often impose limitations on the number of covered sessions per year or per condition. Exceeding these limits shifts the financial burden onto the patient, requiring careful planning and potential exploration of alternative funding options. Understanding these limitations during treatment planning enables informed decisions regarding session frequency and intensity, balancing therapeutic benefit with cost constraints. Furthermore, individual progress and response to therapy can influence the required number of sessions. Faster-than-expected progress might allow for a reduction in sessions and associated costs, while slower progress might necessitate additional sessions and potentially exceed pre-authorized limits, impacting overall expenses. This dynamic interaction underscores the importance of ongoing communication between the patient, therapist, and insurer to adjust treatment plans as needed and address potential cost implications proactively.
Managing the cost of physical therapy requires a comprehensive understanding of the relationship between the number of sessions needed, insurance coverage limitations, and individual treatment progress. Proactive communication with the insurer and therapist regarding treatment plans, pre-authorization limits, and potential out-of-pocket expenses empowers informed decision-making and facilitates a cost-effective approach to rehabilitation. This understanding allows patients to explore alternative funding options, adjust treatment plans as needed, and navigate the complexities of insurance coverage to maximize therapeutic benefit while minimizing financial burden.
Frequently Asked Questions
This section addresses common inquiries regarding the cost of physical therapy with insurance coverage.
Question 1: How does one determine the exact cost of physical therapy with their specific insurance plan?
Contacting the insurance provider directly is recommended. Policy documents often outline coverage details, but direct communication clarifies specific benefits, copay, coinsurance, deductible obligations, and out-of-network coverage details. Benefit summaries and online portals can also provide helpful information.
Question 2: Are there strategies for minimizing out-of-pocket expenses for physical therapy?
Several strategies can minimize costs. Utilizing in-network providers typically results in lower expenses due to negotiated rates. Verifying in-network status before initiating treatment is crucial. Inquiring about package deals or discounted rates for multiple sessions, and exploring alternative funding options like HSAs or FSAs can also reduce costs. Additionally, maintaining detailed records of all treatments and billing statements assists in tracking expenses and identifying potential discrepancies.
Question 3: What happens if required physical therapy exceeds the number of sessions covered by insurance?
When covered sessions are exhausted, several options can be explored. Discussing the situation with the physical therapist may lead to adjustments in the treatment plan to maximize the benefit within the remaining sessions. Negotiating a payment plan with the provider, exploring alternative funding mechanisms, or appealing to the insurance company for additional coverage based on medical necessity are other potential avenues. It is important to understand one’s policy limitations regarding the number of covered sessions.
Question 4: Can one see a physical therapist without a referral from a primary care physician?
Whether a referral is necessary depends on the specific insurance plan. Some plans, such as HMOs, often require referrals for specialist visits, including physical therapy. PPO plans typically do not necessitate a referral, but confirming with the insurer is advisable, as plan specifics vary. Direct access laws vary by state and may allow access to physical therapy without a referral, but insurance coverage still depends on individual plan rules.
Question 5: What recourse is available if a claim for physical therapy is denied by the insurance company?
A formal appeals process is available for denied claims. This process typically involves submitting a written appeal to the insurance company, outlining the reasons for disagreement with the denial. Supporting documentation, such as medical records and treatment plans, should be included. Understanding the appeals process and deadlines outlined in the policy documents is essential. Assistance from the physical therapist or patient advocacy groups can be helpful in navigating this process.
Question 6: Does insurance cover all types of physical therapy modalities and treatments?
Insurance coverage for specific modalities and treatments varies by plan. While many common physical therapy interventions are typically covered, some specialized treatments, such as dry needling or aquatic therapy, may require pre-authorization or may not be covered at all. Reviewing policy documents or contacting the insurer directly clarifies coverage for specific modalities. Understanding these specifics before commencing treatment allows for informed decisions and avoids unexpected expenses.
Proactive engagement with insurance providers and healthcare professionals is essential for managing the cost of physical therapy effectively. Understanding policy details and exploring available resources empowers informed decision-making and facilitates a cost-conscious approach to rehabilitation.
The following section delves into specific examples of various insurance plans and their associated costs for physical therapy.
How Much Does Physical Therapy Cost With Insurance
Navigating the financial landscape of rehabilitative care requires a thorough understanding of the factors influencing cost. Insurance plan types, coverage details, provider networks, and pre-authorization requirements all play a significant role in determining out-of-pocket expenses. From HMOs and PPOs to high-deductible plans, each structure presents unique cost-sharing mechanisms, impacting patient financial responsibility. Copays, coinsurance, and deductibles further shape the overall cost, influencing treatment accessibility and affordability. The choice between in-network and out-of-network providers carries significant financial implications, impacting reimbursement rates and potential balance billing. Pre-authorization requirements introduce an additional layer of complexity, affecting treatment timelines and access to specific interventions. Finally, the number of sessions required, often dictated by the complexity of the condition and individual progress, directly correlates with the cumulative cost of care. Managing these variables effectively necessitates proactive engagement with insurance providers, careful review of policy documents, and open communication with healthcare professionals.
Informed decision-making regarding insurance plan selection, provider networks, and treatment options empowers individuals to navigate the financial complexities of physical therapy effectively. Proactive planning, coupled with a clear understanding of policy benefits and limitations, mitigates the risk of unexpected expenses and facilitates access to essential rehabilitative care. Ultimately, informed financial navigation empowers individuals to prioritize their health and well-being while managing the associated costs responsibly. Access to quality, affordable rehabilitative care remains a critical component of a functioning healthcare system, and understanding the financial intricacies of insurance coverage empowers individuals to navigate this landscape effectively, promoting both individual and collective well-being.